- LOGIN
- MemberShip
- 2026-06-06 10:09:38
- Opinion
- [Reporter’s View] To whom should drug prices be disclosed
- by Jung, Heung-Jun May 27, 2026 04:10pm
- As Korea’s ‘flexible drug pricing contract system,’ which applies dual pricing to pharmaceuticals, goes into full implementation next month, further discussion is needed regarding the scope of disclosure for actual drug prices.Until now, actual drug prices were publicly disclosed through pricing files or reimbursement lists and maximum reimbursement price tables. Going forward, however, information, including products subject to flexible pricing contracts, will only be provided to ‘authorized users,’ such as healthcare institutions.And even authorized users are being cautioned not to use the information for purposes other than calculating pharmaceutical expenses or disclosing it externally.Starting this June, the actual prices of the 12 items listed will not be provided to the general public, who are considered “unauthorized parties.” While there is a difference of 2 to 5 times or more between the listed prices and actual prices of these 12 items, the public reimbursement list only reveals the listed price and whether a flexible pricing contract applies.Considering the purpose of the system, setting outwardly visible prices high in order to maintain competitiveness in international reference pricing systems, such measures may appear understandable.However, as time passes and the number of contracted items increases to the hundreds, information asymmetry is bound to grow. The wider this gap becomes, the more drug price transparency will steadily erode.The government introduced dual pricing primarily to avoid damaging international reference prices when multinational pharmaceutical companies supply medicines to the Korean market or when domestic companies export products overseas.It is difficult to deny that expanding flexible pricing contracts is unavoidable in order to improve access to innovative drugs. It is also clear that the system could strengthen export competitiveness for Korean-developed drugs.However, if preventing damage to reference pricing is truly the main objective of the system, there is no reason to withhold actual pricing information from citizens who wish to know it.Since the dual pricing system differs from risk-sharing agreements in terms of its purpose and contractual methods, is there really a need to keep the actual prices under the flexible pricing system tightly under wraps? If patients, caregivers, researchers, or others are curious about the actual price of a specific drug subject to dual pricing, there should be a way to provide that information.Until now, the general public had no way to access drug prices other than through the reimbursement list. Now that the dual drug pricing system has been implemented, additional methods of access must be provided.Even a passive form of disclosure, such as providing actual pricing information when separately requested by patients or caregivers, should be considered.To prevent the growing information asymmetry from leading to public distrust of drug pricing, the authorities must engage in open deliberation and develop supplementary measures.
- Company
- Potential shift to IgA nephropathy treatment…'Nefecon'
- by Son, Hyung Min May 27, 2026 04:10pm
- The treatment landscape for IgA nephropathy (IgAN) is likely to shift from a focus on conservative management toward targeted therapies that address the disease's underlying cases.While treatments centered on renin-angiotensin system (RAS) inhibitors, aimed at blood pressure control and reduction of proteinuria, have shown limitations, a local immunomodulatory therapy targeting the Peyer’s patches (immune tissue in the ileum) has demonstrated efficacy in reducing proteinuria and protecting renal function, drawing attention to a potential paradigm shift in treatment strategies.On the 26th, Everest Medicines hosted a media session at the Plaza Hotel in Jung-gu, Seoul, to highlight the clinical value of 'Nefecon (micronized budesonide),' a targeted treatment for IgA nephropathy.IgA nephropathy is a primary glomerular disease characterized by the deposition of immunoglobulin A (IgA) within the glomeruli, which induces inflammation and a decline in kidney function. It accounts for approximately 40% of glomerulonephritis cases in South Korea and is known to commonly manifest in individuals in their 20s to 40s who are socially and economically active. Unlike conventional chronic kidney disease (CKD), which frequently occurs in the elderly population in association with diabetes and hypertension, IgAN is distinct in its onset among a relatively younger ages.Although disease progression varies across patients, persistent proteinuria and renal decline carry a high risk of progression to end-stage renal disease (ESRD). The recurrence rate remains at 20% to 60% even after kidney transplantation, and some studies report that the average life expectancy is shortened by approximately 10 years, with a mortality rate roughly twice as high as that of the general population.Jung Pyo Lee, Department of Nephrology, Boramae Medical CenterIn particular, proteinuria and a depressed estimated glomerular filtration rate (eGFR) are recognized as key indicators of disease progression and elevated cardiovascular risk. A British cohort study reported that a considerable number of cases progressed to kidney failure within 10 to 15 years post-diagnosis, demonstrating that patients with higher baseline proteinuria faced a substantially increased risk of ESRD or mortality.Previously, the management of IgA nephropathy has centered on supportive care aimed at slowing the rate of renal deterioration rather than modifying the disease itself. Renin-angiotensin system (RAS) inhibitors designed for blood pressure and proteinuria control. While RAS inhibitors help reduce proteinuria by lowering intraglomerular pressure, they limitations because they do not directly target the underlying pathogenesis.Professor Jung Pyo Lee explained, "While a renal biopsy is vital for a definitive diagnosis of IgA nephropathy, it cannot be practically performed on every patient. Global guidelines recommend a biopsy when proteinuria exceeds 0.5g. However, in real-world clinical practice, RAS inhibitors or SGLT-2 inhibitors are prioritized when proteinuria is under 0.5g. Immunotherapy is considered when proteinuria reaches 1g or more, and there are approximately 10,000 severe patients who would be eligible candidates for Nefecon therapy."Nefecon is a targeted therapeutic designed to modulate the mucosal immune response implicated in the pathogenesis of IgA nephropathy. It is engineered to locally deliver the active drug to the Peyer's patches in the terminal ileum, a recognized primary anatomical site where IgAN originates.Through this mechanism, it downregulates the production of galactose-deficient IgA1 (Gd-IgA1), a key pathogenic biomarker, thereby suppressing abnormal immune cascades. It was explained that while conventional supportive therapies focus mainly on reducing proteinuria and controlling blood pressure, Nefecon distinguishes itself as a 'disease-modifying' approach that modulates the core progression of the disease.The drug-delivery mechanism is also key. It delivers the drug to the target tissue utilizing a dual formulation technology that integrates delayed-release and sustained-release profiles. The budesonide component is specifically designed to minimize systemic exposure, as the vast majority of the active pharmaceutical ingredient is cleared by extensive first-pass hepatic metabolism. According to the presented data, its impact on the HPA axis (hypothalamic-pituitary-adrenal axis) was also relatively limited.Nefecon was designated as the second product under the Ministry of Food and Drug Safety (MFDS)'s Global Innovative Product on Fast Track (GIFT) program in November last year, and it secured approval in the United States in 2021 under the brand name 'Tarpeyo.'Professor Lee explained, "IgA nephropathy features a high proportion of young patients, and the risk of progressing to ESRD fluctuates depending on the severity of proteinuria and renal function decline. It is critical to consider early immunological interventions in high-risk patients."Confirmed effectiveness in proteinuria·renal function protection Professor Jung-ho Shin, Division of Nephrology, Chung-Aug University HospitalThe clinical value of Nefecon was validated through the global Phase 3 NefIgArd study.NefIgArd was a global, randomized, double-blind, placebo-controlled study conducted in patients with primary IgA nephropathy who exhibited persistent proteinuria despite optimized RAS inhibitor therapy. Patients were randomized to receive either Nefecon or a placebo for 9 months, followed by a 15-month observational follow-up period.The clinical results showed that Nefecon significantly reduced levels of the core pathogenic biomarker Gd-IgA1 by 34% compared to the placebo group.Proteinuria was reduced by up to 51.3% at 3 months post-treatment completion, and the preservation effect on eGFR was robustly maintained throughout the 15-month post-treatment follow-up period.Notably, a modeling analysis based on the eGFR slope from the NefIgArd study generated predictive data suggesting that Nefecon treatment could delay the onset of kidney failure and the initiation of dialysis by up to 12.8 years.From a safety perspective, the most frequently reported adverse events (AEs) included peripheral edema, hypertension, muscle cramps, and acne development.Professor Shin stated, "The key feature of IgA nephropathy management lies in long-term preservation of renal function and delaying progression to ESRD, rather than short-term reduction of proteinuria alone. Nefecon is different from conventional conservative therapies as it directly addresses the disease pathogenesis by targeting mucosal immune responses."Professor Shin added, "The clinical data confirmed that the eGFR preservation benefit was sustained even after treatment cessation, and the modeling analysis supported its potential to delay progression to renal failure. It is now time to consider the necessity of earlier therapeutic intervention in high-risk patients."
- Policy
- Boehringer begins drug price negotiations for stroke therapy Metalyse
- by Jung, Heung-Jun May 27, 2026 04:10pm
- Boehringer Ingelheim Korea has entered drug price negotiations with the National Health Insurance Service for Metalyse Inj (tenecteplase), a treatment for acute ischemic stroke in adults.In addition, negotiations have also begun for Meditip’s vasculitis treatment Tavneos Cap (avacopan) and Guerbet Korea’s X-ray contrast agent Elucirem Inj (gadopiclenol).According to industry sources on the 26th, Metalyse 25mg, which was recognized as appropriate for reimbursement by the Drug Reimbursement Evaluation Committee in April, has now entered drug price negotiations, bringing it one step closer to reimbursement listing in Korea.Metalyse, a thrombolytic agent, received domestic approval last October. It garnered attention as the first new treatment option for acute ischemic stroke in approximately 20 years following the indication expansion of Actilyse (alteplase).While Actilyse is a second-generation thrombolytic agent, Metalyse is a third-generation thrombolytic agent with PAI-1 resistance, which inhibits thrombolysis.At the end of last year, the National Assembly also raised the need to introduce third-generation thrombolytics that are already reimbursed overseas, specifically mentioning the rapid reimbursement listing of Metalyse.Meditip’s Tavneos Cap 10mg, which was reviewed alongside Metalyse by DREC in April, is also undergoing price negotiation procedures. At the time, the committee determined the drug was appropriate for reimbursement for the ‘treatment of severe granulomatosis with polyangiitis (GPA) and microscopic polyangiitis (MPA).’However, side effects have become a concern following recent reports of deaths and other adverse events overseas. The Ministry of Food and Drug Safety (MFDS) stated that while the product was supplied to some patients prior to market launch, no adverse event reports had been received. Safety management is expected to influence the price negotiation agreement as well.Negotiations are also underway for Guerbet Korea’s X-ray contrast agents Elucirem Inj and Elucirem Prefilled Syringe Injection, as well as Bracco Imaging Korea’s Vueway Inj.These products had previously been recognized as eligible for reimbursement as “MRI contrast agents for adult and pediatric patients aged 2 years and older,” provided they are accepted at or below the assessed price.As the pharmaceutical company has accepted the term, detailed negotiations with the National Health Insurance Service regarding expected claims costs and related matters are expected to take place thereafter.
- Policy
- DPK "Innovation·eradicate rebates"…PPP "Vaccine safety·NIP expansion"
- by Lee, Jeong-Hwan May 27, 2026 04:10pm
- The Democratic Party of Korea (DPK) and the People Power Party (PPP)Ahead of the June 3 local elections, both the ruling and opposition parties have finalized their core healthcare pledges, focusing on fostering the pharma-biotech industry and driving healthcare innovation.The Democratic Party of Korea (DPK) promised to restructure the domestic pharmaceutical industry, which remains centered on generics, by overhauling the drug pricing system with a strong emphasis on innovation and establishing a fair compensation framework for novel drug development.The DPK also pledged to launch a multi-ministerial cooperation system linking the Ministry of Health and Welfare (MOHW) and the National Tax Service (NTS) to eliminate illegal pharmaceutical and medical device rebates at the source.Granting special judicial police authorizations to the National Health Insurance Service (NHIS) to stop leakages in health insurance finances and dismantle fraudulent profit-making structures was also included in the DPK's official campaign pledges.Meanwhile, the People Power Party (PPP) focused its pledges heavily on expanding vaccine infrastructure closely tied to health security. Leading the introduction of novel pneumococcal vaccines and high-immunogenicity influenza vaccines into the National Immunization Program (NIP) is a key area the PPP plans to champion following the local elections.In the health insurance sector, the PPP made its stance clear on tightening post-hoc management and regulatory controls against illegal medical practices and distribution market distortions that cause leakages in national health insurance finances.These analysis have been made based on the May 26thlocal election manifestos of both major political parties regarding the pharma-biotech and healthcare policies.The DPK, Major transformation of the Pharma-Biotech industry...Implementing an official MOHW-NTS rebate eradication task forceThe DPK placed the structural innovation of the domestic pharma-biotech industry at the forefront of its campaign. The party expressed a strong commitment to introducing an innovation-linked drug-pricing overhaul and a fair compensation framework to shift the domestic pharmaceutical ecosystem away from a generic-centric model toward innovative drugs.Furthermore, the DPK promised to build a state-backed supply chain, including a national contract manufacturing framework for essential medicines such as pediatric drugs and antibiotics, as well as modernizing domestic manufacturing facilities for active pharmaceutical ingredients (APIs).To prevent recurring drug shortages, the DPK’s vision is to establish a collaborative network between the government and pharmaceutical companies to ensure a stable supply of essential pediatric drugs, antibiotics, and vaccines, and to immediately allocate national budget resources to achieve self-sufficiency in APIs, which currently rely heavily on overseas imports.The DPK also declared it would drive efforts to eliminate illegalities in the healthcare market and stop health insurance financial leakage by introducing an SJP system for the NHIS to eradicate illegal non-physician-owned hospitals and implementing periodic, concentrated crackdowns on drug and medical device rebates via MOHW-NTS cooperation.Regarding rebates, the core of the DPK’s pledge is to go beyond one-off enforcement and establish a permanent system capable of executing periodic, intensive crackdowns across the entire illicit transaction architecture, including both rebate providers and intermediaries.To reinforce regional, essential, and public healthcare, the DPK plans to redesign region-specific transfer and referral protocols linking emergency fire services and medical institutions on a city-and-province level, while expanding state compensation liabilities for no-fault medical accidents occurring during essential healthcare delivery.The party also announced the creation of a Medical Accident Review Committee to mitigate upfront judicial risks for essential healthcare physicians, establishing a mutually beneficial safety net.The PPP, Enhancing vaccine safety and expanding NIP...eradicating the causes of 'Emergency Room Hopping'The PPP finalized its central healthcare pledges under the core value of welfare for the underprivileged, placing heavy emphasis on narrowing regional healthcare disparities and substantially improving the emergency medical network.First, the PPP plans to strengthen public healthcare by establishing NHIS-directly operated regional insurer hospitals. This plan aims to ensure that vulnerable regions with weak medical infrastructure can successfully deliver essential medical services, including emergency care, trauma care, obstetric care, pediatric care, and infectious disease response.The PPP also stated it would firmly establish a transfer and referral control tower centered around the Central Emergency Medical Center, and eradicate the core causes of "emergency room hopping" by overhauling clear hospital refusal criteria and transfer guidelines.To ensure ambulances do not wander with patients on board, the party will refine hospital selection guidelines and clear parameters for hospital refusal. Concurrently, the party packaged protective measures for emergency medical staff and strategies to boost definitive care capacity (infrastructure for backup surgery and hospitalization) into its campaign promises.The PPP will also drastically expand support for the National Immunization Program (NIP) to deliver tangible benefits to citizens.To alleviate the medical expense burden on the elderly and underprivileged populations and to realize a health-security framework centered on disease prevention, the party will aggressively increase funding for vaccinations.Specifically, a free shingles vaccination program will be introduced. The NIP support for the shingles vaccine, which resonates most deeply among middle-aged and elderly demographics, will be expanded to include all individuals aged 65 and older.The PPP also pledged to upgrade the vaccine lineup. By introducing novel pneumococcal vaccines and high-immunogenicity influenza vaccines into the NIP, the PPP aims to prevent severe respiratory diseases among senior citizens.
- Opinion
- Bayer accelerates expansion of new drug portfolio
- by Son, Hyung Min May 27, 2026 04:09pm
- Bayer expressed confidence in its growth prospects, highlighting its new drug portfolio –which focuses on cardiovascular and renal disease, oncology, and ophthalmology -- along with next-generation pipelines based on cell and gene therapies.Despite growing pressure from patent expirations and biosimilar competition, the company believes it has established new growth drivers beyond its traditional reliance on blockbuster products. In particular, Bayer identified Korea as a strategic market where the value of innovative therapies can be realized rapidly, while also signaling plans to expand clinical collaborations and startup partnerships.Sebastian Guth, Chief Operating Officer of Bayer PharmaceuticalsSebastian Guth, Chief Operating Officer of Bayer Pharmaceuticals, recently told reporters, “Bayer is entering a new phase of growth based on its strongest-ever portfolio and innovative pipeline. We are focusing on providing first-in-class or best-in-class treatment options in areas with high unmet medical needs.”The global pharmaceutical industry is currently facing a triple burden of patent cliffs, drug pricing pressure, and rising drug development costs, intensifying competition to secure next-generation growth engines. Bayer is no exception, facing the patent expiration of Xarelto (rivaroxaban) and biosimilar competition against Eylea (aflibercept) 2mg.However, Bayer expressed confidence that it can sustain growth momentum through new drug competitiveness in cardiovascular-renal disease, oncology, and ophthalmology, along with future pipelines based on precision medicine and cell and gene therapy.In fact, Bayer secured a total of 5 regulatory achievements last year, including 3 new drug approvals and 2 expanded indications, while also generating positive results from 6 late-stage global clinical trials. Based on this, the company has set goals of restoring growth after 2027 and achieving a 30% operating margin by 2030. According to Guth, Bayer is strategically concentrating on oncology, cardiovascular-renal disease, neurology, rare diseases, and immunology as core therapeutic areas.Kerendia, Nubeqa, and Eylea emerges as growth drivers…“Portfolio transition accelerates”Bayer’s confidence stems from the emergence of new growth products. The company believes Kerendia (finerenone) and Nubeqa (darolutamide) are driving tangible sales growth, while high-dose Eylea (8mg) is establishing itself as a new treatment option in ophthalmology and filling the gap left by existing blockbuster products.Kerendia, in particular, is emerging as a key pillar in Bayer’s integrated cardiovascular-renal treatment strategy. After being approved in Korea for chronic kidney disease associated with type 2 diabetes, Kerendia recently secured an additional indication for heart failure with a left ventricular ejection fraction of 40% or greater. While traditional heart failure treatment has mainly focused on reduced ejection fraction heart failure, treatment options for preserved ejection fraction heart failure have remained relatively limited, and Bayer sees strong potential for changing treatment paradigms in this area.Guth said, “Heart failure with preserved ejection fraction is an area with high unmet medical need in Korea as well. We are focusing on how Kerendia can benefit patients in actual clinical practice.”The prostate cancer treatment Nubeqa is also a core growth driver within Bayer’s oncology portfolio. Nubeqa has expanded its indications in Korea from high-risk non-metastatic castration-resistant prostate cancer to metastatic hormone-sensitive prostate cancer, broadening its treatment scope. Recently, reimbursement criteria for metastatic hormone-sensitive prostate cancer were also established, increasing expectations for improved patient access. Bayer aims to strengthen its leadership in prostate cancer treatment through Nubeqa while also creating future synergies with radiopharmaceutical-based therapies.In ophthalmology, Eylea 8mg was highlighted as a next-generation growth driver. With the aging population and the rise in chronic diseases leading to an increase in patients with age-related macular degeneration and diabetic macular edema, the drug is considered significant because it has the potential to extend treatment intervals, thereby reducing both the financial burden on patients and the workload on healthcare providers. Bayer holds commercial rights for Eylea outside the United States, and the drug is continuing to grow in multiple countries, including Korea.Guth said, “Nubeqa and Kerendia recorded combined growth of 68% last year and exceeded market expectations. Even amid difficult conditions such as the competition brought on by the introduction of Xarelto generics and Eylea 2mg biosimilars, the growth potential of our core products is translating into tangible results.”Accelerating development of cell and gene therapies…”Targeting root causes beyond symptom relief”Bayer positioned cell and gene therapies and precision medicine at the forefront of its future growth strategy. The key concept is “disease modification,” which seeks not merely to manage symptoms but to alter disease progression itself.Parkinson’s disease was presented as a representative example. Bayer is simultaneously developing both cell therapy and gene therapy approaches for Parkinson’s disease.The cell therapy ‘bemdaneprocel’ is a one-time treatment designed to replace lost dopamine-producing neurons and is currently in late-stage clinical development. Meanwhile, the gene therapy ‘AB-1005(ametefgene parvec)’ is being developed to restore neurological function and slow disease progression. Guth explained that these represent entirely new approaches in the field of Parkinson’s disease, where fundamental therapeutic progress has been limited for decades.Guth said, “Parkinson’s disease is an area where there has been little significant therapeutic progress for decades, and Bayer is making meaningful breakthroughs. Because Parkinson’s disease has a severe impact not only on patients but also on their families, we hope both therapies can be developed successfully.”As a next-generation cardiovascular pipeline, Guth highlighted Bayer’s factor XI inhibitor asundexian.Although asundexian faced a temporary development setback for the atrial fibrillation indication, the drug regained momentum by securing positive results in late-stage clinical trials for secondary stroke prevention after strategic adjustments. Bayer expects this drug to set a new standard of care in the future.Guth said, “We experienced setbacks where the research did not meet expectations, but after reviewing the scientific evidence again, we regained confidence in the direction. It is important to learn and stay focused even in the face of failure.”Guth also identified ‘225Ac-PSMA Trillium,’ currently being developed for metastatic castration-resistant prostate cancer, as one of Bayer’s major pipelines.225Ac-PSMA Trillium is a targeted alpha radioligand therapy directed at prostate-specific membrane antigen (PSMA). Bayer plans to expand its prostate cancer treatment strategy by adding next-generation radiopharmaceuticals to the prostate cancer portfolio already built around Nubeqa.“Prostate cancer is an area with high global prevalence and significant unmet medical need. We expect this therapy to bring meaningful changes to patient treatment.”“Korea is a strategic market”…expanding clinical collaboration and startup partnershipsOne of the messages repeatedly emphasized during the interview was the strategic importance of the Korean market. Bayer views Korea not merely as a sales market, but as a global innovation hub with strong scientific capabilities and rapid adoption of innovation.In fact, as of 2025, Korea was found to conduct the second-largest number of investigator-initiated research (IIR) studies worldwide, following the United States.Guth remarked, “Korea’s scientific capabilities are beyond doubt, and the country also possesses outstanding R&D capabilities. There are active efforts aimed not merely at improving existing treatments but at developing first-in-class or best-in-class treatments.”Starting this year, Bayer officially launched “Bayer Co.Lab Connect Seoul,” a collaboration program targeting domestic biotech startups.This program is the Korean version of Bayer’s global life science incubator model previously operated in major innovation hubs worldwide. Rather than simply providing financial support, the program focuses on offering global expertise in regulatory strategy, commercialization, market access, and pricing.“Innovation cannot be achieved alone; Collaboration among academia, startups, and companies is important. Our collaboration with Korea has now moved beyond discussion and entered the execution stage.”At the same time, Bayer plans to use artificial intelligence as a key R&D driver to improve productivity across drug development, clinical research, and pharmacovigilance. The company aims to increase R&D productivity and shorten the time required for innovative therapies to reach patients by 2030 through AI-based technologies.“The advancement of AI-based technologies is fundamentally changing the paradigm of drug development, and research capabilities that seemed impossible only a few years ago are now becoming a reality. Bayer will actively leverage this technological turning point to accelerate R&D innovation and ensure that we achieve our stated goals.”
- Policy
- Two Prolia biosimilar companies receive reimbursement coverage
- by Jung, Heung-Jun May 26, 2026 03:21pm
- Fierce competition is expected as three biosimilar products referencing Amgen’s osteoporosis treatments Prolia (denosumab) and Xgeva (denosumab) enter Korea’s reimbursement list next month.Because more than four companies will now have reimbursement listings for the same products, reimbursement price premiums previously applied to the original products, Prolia and Xgeva, will end.According to industry sources on the 22nd, Prolia biosimilars by HK inno.N and Daewon Pharmaceutical are set to be listed for reimbursement next month.HK inno.N’s Izambia PFS (60mg/1mL), Denbrayce Inj (0.12g/1.7mL), and Daewon Pharmaceutical’s Junod PFS (60mg/1mL) are expected to be newly listed at the lowest reimbursement price among already listed equivalent products.Previously, only three companies had reimbursement listings for denosumab products: Amgen, Celltrion, and Samsung Bioepis. HK Inno.N and Daewon Pharmaceutical will now join the market simultaneously.Amgen’s Prolia is an osteoporosis treatment administered as a subcutaneous injection once every six months that increases bone density and prevents fractures. In Korea, it generates annual sales of approximately KRW 180 billion through co-promotion with Chong Kun Dang.In 2016, Amgen also launched Xgeva (denosumab), which is used to prevent skeletal complications in cancer patients with bone metastases and to treat giant cell tumors of bone.Competition with biosimilars for Prolia and Xgeva began after their substance patent expired in March last year. Currently reimbursed denosumab products include Celltrion’s Stoboclo and Osenvelt, as well as Samsung Bioepis’ Obodence and Xbryk injections. Celltrion’s Stoboclo is co-promoted by Daewoong Pharmaceutical, while Hanmi Pharmaceutical co-promotes Samsung Bioepis’ Obodence.HK inno.N’s Izambia and Daewon Pharmaceutical’s Junod are expected to enter the market at 1KRW 08,290, matching the lowest price currently held by Stoboclo.Meanwhile, Denbrayce, developed by Spain’s mAbxience and introduced to Korea by HK inno.N, will also be listed at the existing lowest reimbursement price of KRW 129,000.Until now, Prolia had maintained price premiums due to having three or fewer listed manufacturers for the same formulation. However, beginning next month, Prolia’s price will be reduced from KRW 123,760 to KRW 108,290, while Xgeva’s price will fall from KRW 195,525 to KRW 171,084.
- Policy
- Abolishing illegal CSO·rebate…under 'National Normalization Project'
- by Kang, Shin-Kook May 26, 2026 03:21pm
- Shim Jong-seop, Director General for Government Operations at the Office for Government Policy CoordinationThe Korean government is launching comprehensive regulatory reforms and monitoring to eradicate illegal rebates and unlawful Contract Sales Organizations (CSOs), which have long been practiced within the pharmaceutical industry, and to rectify abnormal practices in the healthcare sector, such as fraudulent receipt of medical care benefits.The Office for Government Policy Coordination (Director General, Shim Jong-seop) announced on the 22nd that it has finalized 164 initial tasks under the 'National Normalization Project,' an initiative aimed at rectifying deep-seated, abnormal practices and systems across society, and will begin government-wide structural overhauls.This project was coordinated primarily by the 'National Normalization Task Force,' chaired by the Prime Minister, and includes numerous innovation initiatives in the medical and pharmaceutical sectors, led by the Ministry of Health and Welfare (MOHW) and the Ministry of Food and Drug Safety (MFDS).◇ Transparent illegal CSOs and strengthening penalties for healthcare professionals receiving unlawful benefits...enhancing the effectiveness of punishments for pharmaceutical rebatesThe initiative's most prominent aspect involves measures to ensure transparency in the pharmaceutical distribution market. The government has resolved to eradicate illegal CSOs that have exploited legal loopholes to engage in non-compliant expedience. Under the leadership of the MOHW, institutional gaps will be closed with the mainstream, and transparency will be brought to CSO operations. Notably, the government plans to establish new penal provisions targeting healthcare professionals who accept illicit benefits from CSOs, and to launch a comprehensive, large-scale fact-finding investigation.Concurrently, the MFDS will intensively pursue the task of "eradicating pharmaceutical company rebates." The current system penalizes pharmaceutical companies caught providing rebates by suspending sales operations; however, it has been criticized for being ineffective due to rampant loopholes, such as companies pushing out massive sales volumes right before the suspension takes effect. In response, the government will devise measures to significantly improve the enforcement effectiveness of sales suspensions to block illegal rebating at the source.◇ Introducing special judicial police to the NHIS to detect 'fake treatments'... overhauling the reimbursement fee structure for laboratory testingAdministrative measures will also be strengthened to cut off unfair practices and malpractice at the clinical frontline. The MOHW plans to step up proactive prevention of fraudulent medical care benefit claims while introducing a Special Judicial Police system within the National Health Insurance Service (NHIS) to completely root out the leakage of health insurance funds caused by "fake treatments" and "fake patients."Furthermore, the government will completely overhaul the 'health insurance reimbursement fee structure for outsourced laboratory testing,' which has previously been flagged as a threat to patient safety. New differentiated reimbursement fees for outsourcing and consigned testing institutions will be established. Accreditation standards for consigned laboratories, quality-linked incentive systems, and penalty criteria will be upgraded to enhance testing quality and guarantee patient safety.The Korea Disease Control and Prevention Agency (KDCA) will also target abnormal non-profit organizations that may have suffered from lax oversight, identifying financial vulnerabilities and enhancing accounting transparency by upgrading systems and strengthening the management of secure media and assets.◇ Detecting 'Fake Ambulances' in Real-Time...Introducing GPS-Based integrated management 'Fake ambulances,' which have provoked public outrage due to incidents involving celebrities riding in them or other forms of unauthorized private use, are set to disappear. The government will introduce a GPS-based, real-time integrated operations management system for ambulances and rationalize emergency transport and treatment fees to improve oversight efficiency and establish a stable operational environment.In addition, to ensure the golden-hour for severe emergency patients, the National Fire Agency (NFA) and the MOHW will collaborate to extensively upgrade the patient transfer network between fire services and medical institutions based on regional medical resource availability.Shim Jong-seop, Director General for Government Operations at the Office for Government Policy Coordination, emphasized, "This National Normalization Project is not a one-off event but a systematization of the core duties that the government must perform." Shim added, "We will rigorously manage the process to deliver clear results that the public can see."
- Company
- Pulsed field ablation gains reimbursement in Korea
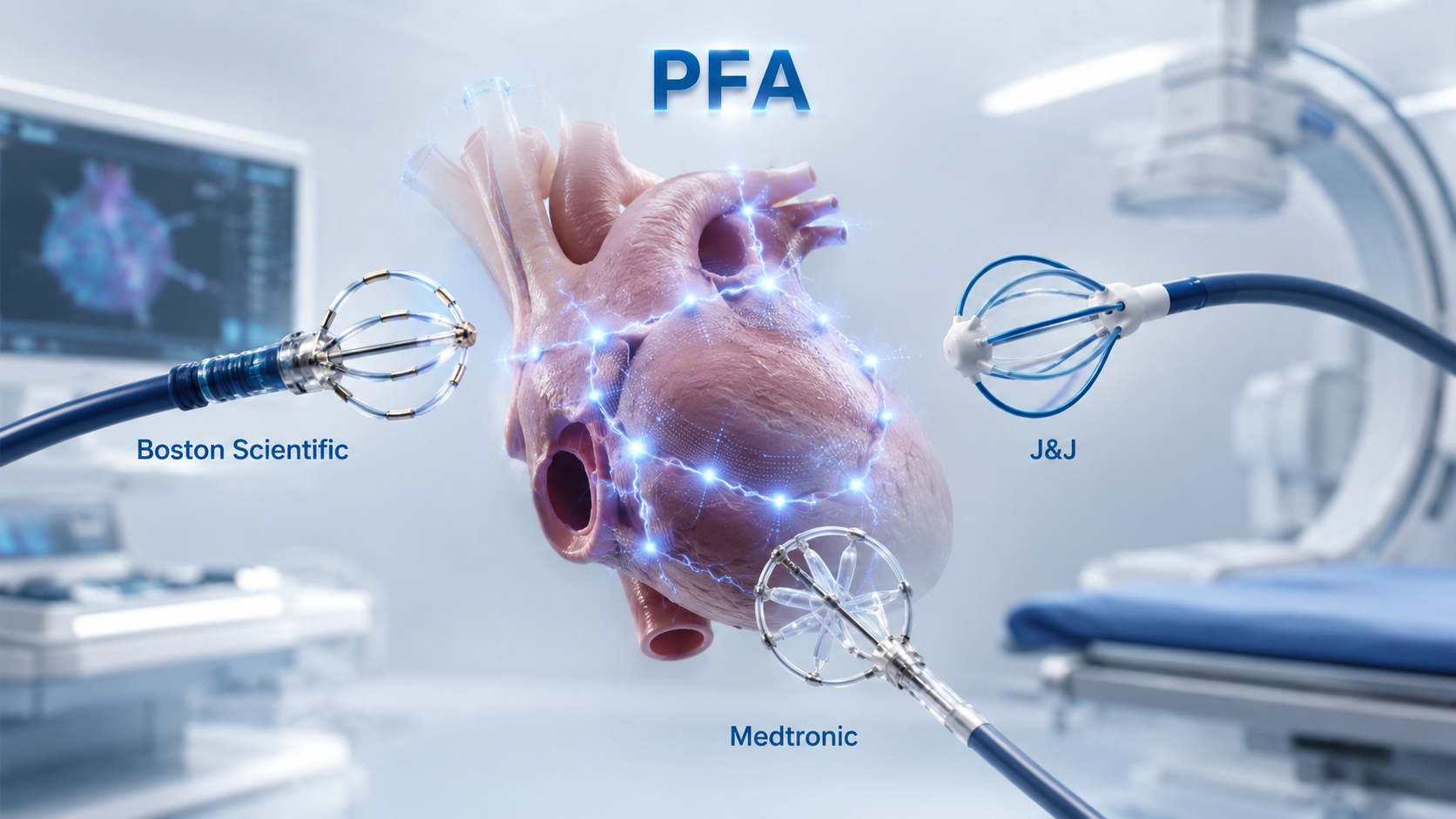
- by Hwang, byoung woo May 26, 2026 03:21pm
- Reference Material (AI-generated image)The atrial fibrillation ablation market has entered a full-scale competition following reimbursement coverage for pulsed field ablation (PFA).PFA has been garnering attention as a next-generation technology capable of replacing existing radiofrequency and cryoablation procedures, but its adoption was limited due to non-reimbursement barriers. However, with national health insurance coverage beginning in May, patient access has improved, and market conditions are changing.In particular, because the reimbursement applies not to a specific company’s product but to the ‘PFA procedure’ itself, Boston Scientific, Johnson & Johnson (J&J), and Medtronic are all expected to compete under the same regulatory framework.Reimbursement marks a turning point in the market... Will PFA adoption accelerate?PFA is an ablation procedure that uses high-voltage electric fields to selectively damage myocardial cells. Unlike conventional radiofrequency ablation or cryoablation, which rely on heat, PFA is considered a next-generation atrial fibrillation treatment because it can reduce damage to surrounding tissues.In particular, its ability to reduce the risk of complications, such as esophageal injury, phrenic nerve injury, and pulmonary vein stenosis, which were concerns with traditional thermal ablation, is cited as a key strength. Combined with the potential for shorter procedure times, the shift to PFA is already progressing rapidly in the global market.According to a report by the Korea Health Industry Development Institute, Korea’s PFA market is expected to grow from approximately USD 31 million in 2024 to around USD 53 million by 2029, representing a compound annual growth rate of 11.1%.The global PFA market is projected to expand from approximately USD 1.53 billion in 2024 to about USD 9.25 billion by 2029.In practice, even during the non-reimbursed stage, some major tertiary hospitals had already accumulated experience using PFA. According to the report, Severance Hospital introduced PFA at the end of 2024 and has been actively using it since 2025.Out of roughly 1,000 total atrial fibrillation ablation procedures currently performed, about 350 are now conducted using PFA, and the hospital expects more than 70% of all procedures to eventually transition to PFA.Ultimately, while PFA was previously used only on a limited basis depending on whether patients had out-of-pocket insurance coverage, its reimbursement coverage is expected to reduce cost barriers and position PFA as a major treatment option for atrial fibrillation ablation.Market Size and Growth of Korea's PFA Market (Reconstructed AI image of Korea Health Industry Development Institute's report)Boston Scientific’s early approval advantage…J&J focuses on integration, Medtronic on expandabilityAccording to the medical device industry, Boston Scientific currently holds the leading position in the early competitive landscape.Boston Scientific’s Farapulse PFA platform became the first medical device approved in Korea for PFA when it received Ministry of Food and Drug Safety approval in September 2024.Boston Scientific emphasizes that, in connection with the new reimbursement coverage, it possesses both the “Farawave PFA Catheter,” capable of two-dimensional visualization, and the “Farawave NAV PFA Catheter,” which enables three-dimensional visualization of treatment sites.Farapulse’s strengths lie in its early approval and accumulated clinical evidence. According to the company, Farapulse has built up safety and efficacy data through studies such as the ADVENT trial, which directly compared it with thermal ablation, and the MANIFEST-17K registry, which analyzed real-world clinical outcomes in more than 17,000 patients.Its competitor, Johnson & Johnson, is promoting a different type of competitiveness through Varipulse. The Varipulse system is a three-dimensional PFA treatment solution consisting of the Varipulse catheter, TruPulse generator, Carto3 3D mapping system, and Vizigo Steerable Sheath.Its key advantage is integration. Varipulse is designed to integrate with J&J’s electroanatomical mapping system, Carto 3. Because confirming catheter position, visualizing cardiac structures, and identifying lesion locations are increasingly important during PFA procedures, integration with mapping systems may become an important factor in hospital purchasing decisions.Being somewhat of a late entrant in Korea, Medtronic is establishing a competitive presence in terms of expandability.Medtronic’s PulseSelect PFA system received U.S. FDA approval in December 2023 for the treatment of paroxysmal and persistent atrial fibrillation. The company is expected to leverage the fact that PulseSelect was the first PFA system approved by the FDA, along with its global clinical usage experience.Another differentiating point for Medtronic is its future product lineup. Through products such as the dual-energy Affera Mapping and Ablation System, which combines pulsed field and radiofrequency energy, and the Sphere-9 Catheter, the company is pursuing a strategy of expanding treatment areas beyond atrial fibrillation into atrial flutter and ventricular tachycardia.KHIDI Report (AI image reconstruction)Competition lies in hospital workflows rather than productsFollowing reimbursement listing for PFA, market competition is likely to unfold not as a one-sided dominance by a specific company, but rather as a diversification of selection criteria among individual hospitals.Atrial fibrillation ablation procedures are not determined by a catheter alone. Mapping systems, imaging equipment, physician expertise, existing hospital equipment infrastructure, training support, long-term clinical data, and cost structures all play important roles. As a result, preferred platforms may vary from hospital to hospital.For example, hospitals prioritizing early adoption experience and accumulated clinical evidence may favor Boston Scientific’s Farapulse, while hospitals already operating electrophysiology workflows centered on the Carto3 system may choose J&J’s integrated Varipulse solution.Hospitals focusing on future technologies and expandability of indications may instead see Medtronic’s long-term product lineup as more competitive.Nevertheless, the general consensus is that as PFA becomes mainstream, the atrial fibrillation ablation market has entered a full-fledged transition phase.Whereas the technology was previously used mainly by select patients and leading hospitals, patient accessibility and hospital adoption potential are now expanding simultaneously.As a result, while domestic approval and early adoption were previously the key competitive factors, post-reimbursement competition is expected to depend increasingly on real-world experience, interoperability with existing hospital equipment, procedural training, data accumulation, and the speed of follow-up product introductions.A medical device industry official said, “In overseas markets such as the United States, PFA is already rapidly establishing itself as the standard of care. With reimbursement now improving patient access in Korea as well, the transition toward PFA driven by procedural efficiency and safety is expected to accelerate further.”
- Company
- Varying performance levels of medical imaging AI companies
- by Hwang, byoung woo May 26, 2026 03:21pm
- AI-generated imageDomestic medical imaging artificial intelligence (AI) companies reported varying performance in their first-quarter results, even as they posted losses.While attention was previously focused on whether these companies could generate any sales during the initial stages of commercialization, the market is now asking "How do these companies make money?"Consequently, the attention is on the Q1 2026 performance is not top-line sales rankings, but rather the specific channels through which sales is generated. Performance divergence among medical imaging AI companies is accelerating, depending on factors such as overseas commercialization channels, integration into domestic institutional healthcare frameworks, and volume-based recurring revenue streams.Positive indicators in overseas·recurring revenue…Lunit·Coreline Soft differentiating factorsLunit recorded revenue of KRW 24.0 billion for the first quarter of 2026, a 25% increase compared to the KRW 19.2 billion recorded in the same period last year. Concurrently, its operating loss narrowed from KRW 20.8 billion to KRW 13.6 billion, demonstrating increased revenue alongside a reduction in losses.The most critical indicator in Lunit’s performance is its overseas revenue. According to the company's Q1 financial data, international sales reached KRW 23.2 billion, a 29% increase from KRW 17.9 billion in the prior-year period, accounting for a 97% of total revenue.Domestic medical AI markets are highly susceptible to institutional and regulatory factors, such as New Medical Technology Assessments, non-reimbursement status, and reimbursement rates. Conversely, Lunit has successfully established a structure in which the vast majority of its quarterly revenue is secured through global distribution channels.By business segment, cancer screening remains the primary growth driver. Software revenue from Lunit's cancer screening segment totaled KRW 21.3 billion in Q1, accounting for approximately 89% of total revenue.Although its cancer treatment decision-support segment, which includes Lunit SCOPE, is emerging as a new growth vector, the core revenue generator as of Q1 2026 remains the cancer screening business, which includes diagnostic imaging assistance and breast cancer screening software.However, challenges persist on the bottom line. While its operating loss narrowed, the company still posted a KRW 13.6 billion deficit in the first quarter. Although an improving trend in profitability has been confirmed, further revenue expansion and disciplined cost management are required to achieve a turnaround to operating profitability.Comparison of 2025-2026 first quarter revenue of major medical imaging artificial intelligence (AI) companies (unit: KRW 100 million/source: quarterly reports). Lunit, Vuno, Deepnoid, Coreline Soft, and JLK.Coreline Soft, while not yet achieving Lunit's massive exterior performance, showed other positive indicators in its revenue structure.Coreline Soft recorded consolidated revenue of KRW 1.3 billion in the first quarter of this year, representing an approximate 44% increase year-over-year.Out of this total, overseas revenue amounted to approximately KRW 800 million, representing 62.4% of its overall business. This was the first time the company's international revenue share has exceeded 50%.The expansion of its recurring revenue stream is also noteworthy. The company announced that the share of recurring revenue derived from volume-based utilization, term licenses, and software maintenance agreements reached 49.1% in Q1, climbing roughly 10 percentage points from 38.9% in the prior-year period.Specifically, volume-based pay-per-use revenue surged by 319.7% year-over-year. This indicates that the business model of medical AI companies is successfully pivoting from one-off, on-premise deployments and perpetual license sales toward a framework dynamically tied to actual utilization rates and diagnostic screening traffic.This structural shift is closely aligned with international national screening initiatives. According to Coreline Soft's documents, the company secured 11 new hospital contracts in Germany during Q1 alone, surpassing its entire annual total of 10 new contracts in Germany for the previous year within a single quarter.Coinciding with Germany’s statutory health insurance reimbursement coverage for low-dose CT (LDCT) lung cancer screening, demand for AI-driven diagnostic reading, quality control, and longitudinal tracking systems is poised for further expansion.Ultimately, Lunit leveraged international revenue to establish a quarterly baseline of over KRW 20 billion, while Coreline Soft signaled a clear structural pivot toward recurring revenue streams despite its smaller absolute volume. The former differentiated itself through scale, and the latter through its business model structure.Vuno shows high reliance on DeepCARS…performance staggers due to regulatory variablesIn the case of Vuno, the company had previously achieved record-high consolidated annual revenue of KRW 34.8 billion last year, growing 35% year-over-year, and successfully narrowed its operating loss by 60% down to KRW 4.9 billion through aggressive cost-optimization initiatives.Performance was led by its flagship product, DeepCARS, an AI-driven cardiac arrest prediction medical device, which generated KRW 25.7 billion in revenue, representing an approximate 18% year-over-year increase.However, its momentum slowed in the first quarter of 2026, with revenue dipping 16% quarter over quarter to KRW 6.0 billion.The company explained that this temporary revenue fluctuation occurred as DeepCARS navigated the New Medical Technology Assessment process, coinciding with the expiration of its assessment deferral window.Vuno’s challenge lies in the high concentration of its core revenue stream in domestic DeepCARS sales.Although Vuno has designated the US commercial launch of DeepCARS as its top strategic priority, a fully realized revenue stream backed by US regulatory clearance and insurance reimbursement has not yet materialized. Consequently, Vuno's Q1 financial performance remained dependent on domestic DeepCARS sales and the progress of the domestic New Medical Technology Assessment procedures.While market expansion is anticipated once the regulatory assessment process is finalized, establishing and diversifying commercial pipelines in global markets remains an urgent, ultimate objective.AI-generated imageDeepnoid·JLK, In a transitional phase prior to scaling revenue volumeDeepnoid generated only KRW 7.5 billion in annual revenue, falling significantly short of its previously guided revenue forecasts.Deepnoid attributed this discrepancy to slower-than-expected expansion in medical AI adoption, delays in securing health insurance reimbursement pricing and international regulatory clearances, and intensifying competition from incumbent PACS (Picture Archiving and Communication System) vendors.Furthermore, Deepnoid disclosed that it halted the standalone commercialization of DEEP:PHI, citing diminished differentiation for platform-type business models following the advent of generative AI.Its revenue for the first quarter of 2026 amounted to approximately KRW 400 million. Even within this figure, the company relied heavily on its industrial AI division (roughly KRW 300 million) rather than its core medical AI segment (which brought in just KRW 57.75 million).As operating deficits widened due to increased fixed costs associated with R&D scaling and expert talent acquisition, the company’s top priority has shifted to proving the self-sustainability of its medical division. This hinges on successfully anchoring its cerebral aneurysm solution, "DEEP:NEURO," within the domestic non-reimbursement market.JLK is actively driving market entry into the non-reimbursement sector for its pipeline expansion, including its large vessel occlusion (LVO) detection solution, "JLK-LVO", starting with the current non-reimbursement prescriptions of its ischemic stroke solution, "JLK-DWI."However, to overcome the limitations of a constrained domestic market, the company is committing substantial capital to establishing international commercial networks via its wholly owned subsidiaries in the United States (JLK USA INC.) and Japan (JLK Japan, Inc.).Both JLK USA and JLK Japan reported zero revenue in the first quarter, posting net losses of approximately KRW 100 million each. Because these international subsidiaries have yet to generate meaningful top-line contributions, the company is currently in a wait-and-see window to determine whether these infrastructure investments will successfully translate into global financial performance.A medical device industry employee stated, "With digital health companies that have secured insurance reimbursement pricing recently reporting robust financial metrics, pressure to perform is intensifying for medical imaging AI firms as well. We have entered a stage where regulatory clearance or initial hospital adoption alone no longer satisfies market evaluation. The core mandate now is establishing a commercial architecture that translates into sustainable, predictable revenue."
- Company
- Will reimbursement of CDK4/6 inhibitors finally be expanded?
- by Eo, Yun-Ho May 26, 2026 03:21pm
- The decisive moment for expanding reimbursement coverage of CDK4/6 inhibitors in early breast cancer is approaching.According to industry sources, Eli Lilly Korea’s Verzenio (abemaciclib) and Novartis Korea’s Kisqali (ribociclib) are expected to be submitted this week to the Health Insurance Review and Assessment Service’s Cancer Disease Deliberation Committee.The specific indication under consideration for reimbursement expansion is “adjuvant therapy for patients with HR-positive (hormone receptor-positive)/HER2-negative stage II and III early breast cancer at high risk of recurrence.”Although the two drugs share the same mechanism of action, their situations differ somewhat. Verzenio is making its fourth attempt before the reimbursement committee, while Kisqali is being reviewed for the first time. The reimbursement expansion application for Kisqali was filed by the pharmaceutical company itself, whereas the application for Verzenio was submitted by the Breast Cancer Subcommittee of the Korean Society of Medical Oncology.Verzenio faced difficulties in being reviewed by CDDC from its first attempt for early breast cancer. After a long wait of 6 months after submitting the reimbursement application, it was finally reviewed by CDDC in May 2023, but the result was “reimbursement criteria not set.” Five months later, in October, Lilly resubmitted the reimbursement application to HIRA, and in March and July last year, it was submitted to CDDC for review, resulting in the same outcomes.The overall survival (OS) data was cited as the primary reason for Verzenio’s failure to secure expanded coverage. However, with Verzenio now securing OS data, expectations are rising for this CDDC review.In contrast, Kisqali, which is making its first attempt, has not yet secured OS data. While an improvement in OS is foreseeable, there is no direct supporting data available yet.Invasive disease-free survival (iDFS) is regarded as a clinically meaningful surrogate endpoint strongly correlated with OS in early breast cancer due to the disease characteristics, and Kisqali demonstrated encouraging results in the NATALEE study.Although the two drugs share the same mechanism, their differing circumstances make it noteworthy to see what outcomes the two drugs will yield at the CDDC review.