- LOGIN
- MemberShip
- 2026-06-06 10:09:38
- Company
- Eli Lilly Korea's CEO transition…Seiya Komatsu expected to be named
- by Eo, Yun-Ho May 18, 2026 09:11am
- The CEO of Eli Lilly Korea is expected to be replaced.According to industry sources, Eli Lilly has appointed Seiya Komatsu as the new CEO of its Korean affiliate.The appointment comes as the term of the current president, John Bickel, is set to end.As of the end of this coming July, John Bickel, who took office in August 2024, is scheduled to be promoted to a position at Eli Lilly's global headquarters.The newly appointed CEO, Seiya Komatsu, is an industry expert who joined Eli Lilly Japan as a sales representative in 2012 and has acquired diverse experience across various roles, including brand marketing manager, business transformation consultant at global headquarters, and sales manager for the Texas region in the United States. Currently, Komatsu serves as Vice President and Head of the Neuroscience Business Unit at the Japanese affiliate.Meanwhile, Eli Lilly supplies pharmaceuticals across various therapeutic areas, including oncology and autoimmune diseases, as well as its obesity treatment, 'Mounjaro.' Notably, Mounjaro recorded global sales of USD 8.7 billion (approximately KRW 12.7 trillion) in the first quarter of this year, surpassing MSD's 'Keytruda,' ranking No.1 in global pharmaceutical sales performance.
- Policy
- Price cuts on existing drugs divided into two phases
- by Jung, Heung-Jun May 18, 2026 09:11am
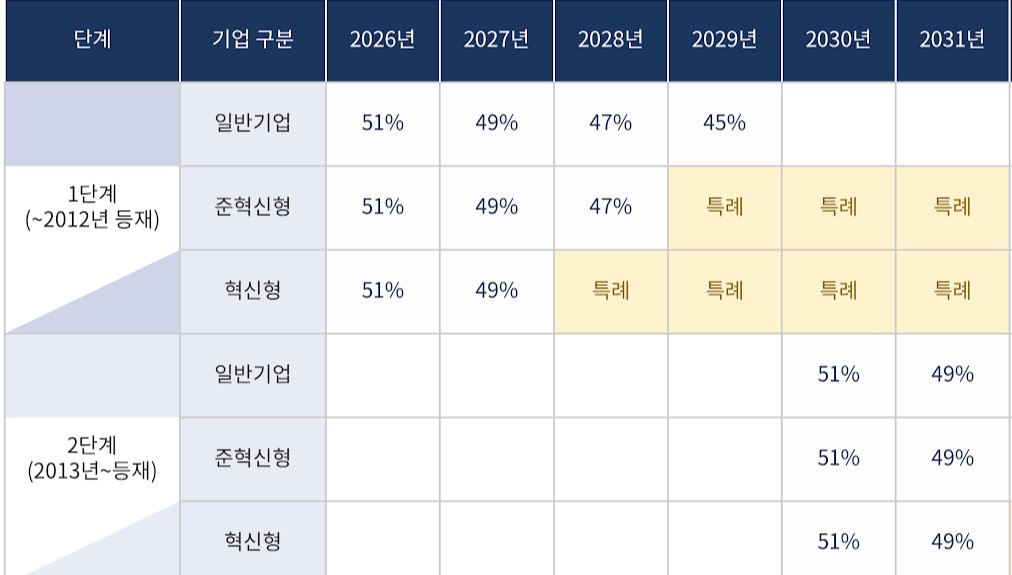
- As the government proceeds with planned pharmaceutical pricing system reforms, follow-up discussions are expected regarding specific classification criteria for price reductions of pre-listed drugs.Key issues include how to distinguish between first-phase and second-phase price reductions for two- and three-drug combination products, as well as how and when later bioequivalence testing should be reflected in drug price reductions.According to industry sources on the 15th, specific criteria for price reductions on pre-listed drugs have not yet been finalized. Discussions on price reductions for pre-listed drugs were not properly addressed during the working-level consultative body meeting between the government and the pharmaceutical industry held in late April.Previously, the Health Insurance Review and Assessment Service (HIRA) decided to divide drugs into two groups based on their listing date in 2012. Price reductions for ingredients listed before 2012 will begin immediately within this year, while reductions for Phase 2 drugs, listed after 2012, will begin in 2030.The timing of implementation differs depending on whether a product is classified into the first or second phase of existing drug price cutsHowever, opinions remain divided regarding the classification of combination products. If the individual ingredients making up a combination drug belong to both Phase 1 and Phase 2 groups, authorities must determine at which timing the combination product itself will face price reductions.The government has stated that if even one ingredient in a combination product was listed before 2012, the combination drug would be classified as a Phase 1 drug.However, there are many issues that require consultation with the industry, such as how to handle cases where even a single ingredient retains a patent or has PMS remaining.Another key issue is how to reduce prices for drugs that failed to meet required standards due to a lack of bioequivalence testing. The reduction rate under the differentiated standards system has been increased from 15% to 20%.For example, if a product price was lowered to 45% and bioequivalence testing was not conducted, it would fall further to 36%. If a rate of 49% is applied, being a product from an innovative pharmaceutical company, it would become 39.2%, while applying a quasi-innovative rate of 47% would drop the price to 37.6%.Since price reductions for pre-listed drugs are implemented over a 10-year period, including a grace period, it is also important to determine how to reflect the results if bioequivalence testing is conducted during that period.In particular, since Phase 2 drugs will only begin facing reductions in 2030, some pharmaceutical companies may attempt to protect reduction rates by conducting bioequivalence studies.Accordingly, industry players are expected to argue that satisfying bioequivalence requirements by the final year converging toward the calculation rate should still qualify as meeting standard requirements.
- Policy
- Calculation rate for generic drug prices set at 45%
- by Lee, Jeong-Hwan May 18, 2026 09:11am
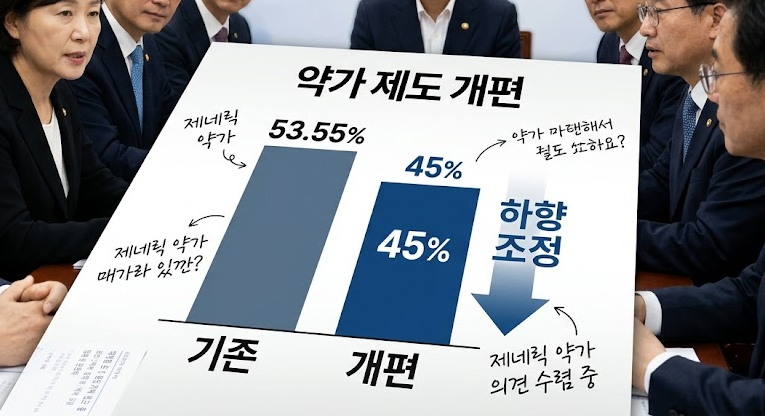
- The government has announced that a drug pricing reform plan, which cuts the drug price calculation rate for currently listed generics from 53.55% to 45%, will take effect on August 1st.The reform plan also includes improvements regarding the management of multiple-listed items, drug price calculations for transfers and acquisitions, support criteria for drugs subjected to market withdrawal, and criteria for semi-innovative pharmaceutical companies.On the 14th, the Ministry of Health and Welfare (MOHW, Minister Jung Eun-kyeong) issued a public notice for the partial amendment to the "Criteria for determination and adjustment of drugs." The ministry plans to finalize the amendment after gathering public feedback by July 13th.The implementation date for the drug pricing reform specified in the amendment notice is August 1st. The government announced that it will gather opinions until July 13th.Generic drug price calculation rate 45%....products failing to meet requirements will be priced below 36%First, the drug price calculation rate for currently listed generics will be reduced from 53.55% to 45%. The calculation rate applied to generics that fail to meet the baseline requirements will also be reduced from 85% to 80%.The baseline requirements for the drug price include whether the company conducted an independent bioequivalence test and whether it used registered drug master file (DMF) ingredients.Generics that meet all baseline requirements will be priced at 45%, those meeting some requirements will be priced at 36%, and products failing to meet any requirements will be priced at 29%.In the case of tiered pricing, the price will be cut once the number of listed items with the same formulation exceeds 13. This is a tighter restriction compared to the current threshold of 20 or more items.If the sum of the newly applied product and the number of currently listed items with the same formulation exceeds 14, the upper limit price will be fixed at 85% of the calculated amount once the price premium period ends.Innovative pharmaceutical companies, semi-innovative pharmaceutical companies, and supply-stabilizing leading pharmaceutical firms will receive preferential drug pricing. Among drugs that meet all baseline requirements, items from innovative pharmaceutical companies will receive a 60% price premium. The premium rate for items from semi-innovative pharmaceutical companies or supply-stabilizing leading pharmaceutical companies will be 50%.Definitions for semi-innovative pharmaceutical companies and supply-stabilizing leading pharmaceutical companies were also established. A supply-stabilizing leading pharmaceutical company is defined as a firm whose ratio of low-profit prevention support drugs, or the ratio of billing amounts among its listed drugs, is 20% or higher.Regarding transfers and acquisitions, the government decided to restrict the succession of existing upper limit prices for items involving a change in a manufacturer's status, excluding inheritance or mergers. Even if a generic item that maintains a high drug price is acquired, the recalculated drug price will be applied from the time of the transfer and acquisition.This regulation is designed to block back-door strategies to evade drug price cuts by purchasing items that maintain high prices.Support for drugs facing production discontinuation will be strengthened. The designation criteria for these drugs are KRW 578 for oral medications, KRW 44 per minimum unit for oral liquids, KRW 3,080 for external preparations, and KRW 5,783 for injections.A new premium clause was also created for pharmaceutical companies that have contributed to supply stabilization. The premium evaluation items include the track record of stable supply fulfillment, national essential medicines, single-listed medicines, low-priced medicines, the use of domestically produced raw ingredients, an annual billing amount of less than KRW 500 million in the previous year, treatments for statutory infectious diseases, and infectious disease crises or urgent supply shortage situations.Price-volume linkage system officiated…implemented on April 1st and October 1st of each yearThe timing of drug price cuts resulting from the price-volume linkage system and the expansion of the scope of use has been unified. The amendment specified that the ex officio adjustment of the upper limit price of drugs will be implemented on April 1st and October 1st of each year, unless there are special circumstances.In addition, a basis was established for pharmaceutical companies to refund the increased expenditure on health insurance incurred during the implementation grace period to the National Health Insurance Service if a drug price adjustment is issued at a time other than the regular implementation date.Meanwhile, the MOHW plans to implement the announced reform plan on August 1st. Regulations related to the regularization of the price-volume linkage will apply starting in January of next year (2027). The first regular drug price adjustment will take effect on April 1st, 2027.
- Product
- Regulatory sandbox for OTC drug vending machines revisited
- by Kim JiEun May 18, 2026 09:11am
- Discussions surrounding a regulatory sandbox pilot exemption for “smart vending machines for over-the-counter essential medicines,” which has remained unresolved for years, have recently resumed. With the expert committee under the Ministry of Trade, Industry and Energy’s Regulatory Exemption Deliberation Committee convening again after about 2-3 years, debate over permitting unmanned sales of OTC essential medicines appears to be reigniting.In particular, it is reported that a heated debate ensued during this meeting, with the industry strongly advocating for the pilot exemption by emphasizing the need for installation in medically underserved areas and technological advancements, while the Korean Pharmaceutical Association and the Ministry of Health and Welfare clearly stated their opposition, as they have in the past.According to multiple sources on the 15th, the Ministry of Trade, Industry, and Energy held the “5th Expert Committee Meeting of the Regulatory Rationalization Committee” at the end of last month to discuss a proposal for a pilot exemption regarding smart vending machines for over-the-counter medicines.This marked the first reopening of discussions on the issue in approximately two to three years after deliberations had effectively been suspended. It was reported that attendees included representatives from the Korean Pharmaceutical Association, the Ministry of Health and Welfare, the Ministry of Trade, Industry and Energy, the applicant company Urban Sharing Economy, as well as legal and academic experts.The core of this proposal is to allow the sale of over-the-counter medicines through unmanned smart vending machines. Previously, the company had applied for a regulatory sandbox, proposing a smart vending machine model that integrates biometric authentication and remote control systems based on 13 over-the-counter medication items currently sold at convenience stores.At the time, the Korean Pharmaceutical Association strongly opposed the proposal, expressing concern that the unmanned sale of medications could expand gradually following the approval of video-based dispensing machines. As discussions failed to reach a conclusion for an extended period, the matter remained effectively on hold.However, during this latest meeting, the Ministry of Trade, Industry, and Energy reportedly emphasized that “a conclusion needs to be reached on the issue that remained unresolved for 5 years,” strongly advocating for the necessity of a pilot exemption.It is reported that the company presented an additional plan to focus installations on medically underserved areas, such as remote islands and mountainous regions, where access to pharmacies and convenience stores is limited, in addition to its existing proposal.It is also reported that they emphasized the stability of the technology, noting that biometric authentication and control systems had been further refined during the period when discussions were suspended.On the other hand, the Korean Pharmaceutical Association and the Ministry of Health and Welfare reaffirmed their opposition. They reiterated the existing logic that pharmaceutical sales should be premised on face-to-face medication guidance and safety management systems, and that expanded unmanned sales could lead to misuse and safety concerns.During the meeting, a heated debate reportedly continued over whether to proceed with the pilot exemption.An official who attended the meeting stated, “Toward the end of the meeting, the atmosphere even reached the point where we were about to decide on proceeding with the exemption via a show of hands, but the debate between supporters and opponents continued for a long time. Ultimately, the Ministry of Trade, Industry and Energy decided to refer the matter to the next expert committee.”At the meeting, ministry officials reportedly stated that a sixth expert committee meeting would be convened within 1-3 months to make a final decision on whether to proceed with the pilot exemption.Within and outside the industry, some observers believe a partially positive sentiment toward the project is forming inside the Ministry of Trade, Industry, and Energy. In fact, several participants at the meeting reportedly expressed opinions sympathetic to the need for pursuing the pilot project.However, given the continued strong opposition from the Ministry of Health and Welfare and pharmacy organizations, as well as the possibility that allowing unmanned pharmaceutical sales could expand into a broader social controversy, significant conflict is expected before a final conclusion is reached.
- Opinion
- ‘Need to change perceptions on menopausal hormone therapy’
- by Son, Hyung Min May 18, 2026 09:11am
- With the US Food and Drug Administration (FDA) recently removing the Black Box Warning imposed on menopausal hormone therapy (MHT) products, the likelihood of a shift in perception is growing within Korea’s obstetrics and gynecology clinical field.While there has long been a strong tendency to avoid treatment due to concerns about the risk of breast cancer and cardiovascular disease, there is now a growing emphasis on the need for personalized treatment that takes into account the patient’s age, time of menopause, and risk factors.In particular, experts pointed out that the findings of the US Women’s Health Initiative (WHI) study had been excessively generalized to women in early menopause, and stressed that the long-term health benefits of early treatment, such as the prevention of cardiovascular disease, osteoporosis, and dementia, should also be considered.In a recent meeting with DailyPharm, Eun Sil Lee, Professor of Obstetrics and Gynecology at Soonchunhyang University Seoul Hospital, and Tae-Hee Kim, Professor of Obstetrics and Gynecology at Soonchunhyang University Hospital Bucheon, assessed that this FDA action could serve as an opportunity to fundamentally redefine existing perceptions of MHT, going beyond the mere removal of warning labels.(From the left) Professor Eun Sil Lee (Obstetrics and Gynecology, Soonchunhyang University Seoul Hospital) and Professor Tae-Hee Kim (Obstetrics and Gynecology, Soonchunhyang University Hospital Bucheon)The two professors particularly pointed out that although the 2002 WHI study was conducted on a patient population different from actual women in early menopause, the findings were subsequently applied uniformly to women of all ages, creating excessive fear toward hormone therapy.Based on the study results, the FDA introduced Black Box Warnings for MHT products in 2003. Following this, concerns over breast cancer, cardiovascular disease, and dementia risks spread rapidly, causing hormone therapy prescriptions to decline sharply worldwide. However, as more age-specific and menopause timing-based reanalyses accumulated in recent years, the FDA initiated procedures last November to remove the warning.Experts point out that the WHI study results were overgeneralized.The WHI study included women with an average age of 63, many of whom already had a significant number of risk factors for cardiovascular disease. Another limitation cited is that the study used a combination of hormones that is no longer widely used today. Subsequent age-specific analyses showed that for women who began treatment within 10 years of menopause, particularly those in their 50s, there was no clear increase in the risk of cardiovascular disease or dementia, and some studies even suggested possible preventive effects.In practice, MHT has long been used as a representative menopause management therapy, having been proven effective not only in alleviating menopausal symptoms such as hot flashes, sleep disturbances, and depression but also in preventing osteoporosis. However, following the publication of the WHI study, concerns about breast cancer risk spread rapidly, leading to a strong trend in Korea toward discontinuing or avoiding the treatment.Recently, there has been growing discussion that MHT should be reevaluated from a “well-aging” perspective, one that goes beyond simple symptom management to include cardiovascular health, osteoporosis prevention, and the management of healthy life expectancy. As life expectancy increases and women spend longer periods living after menopause, experts argue that both risks and benefits of treatment should be evaluated in balance.The two professors emphasized, “MHT should not be oversimplified solely in terms of breast cancer risk. It should instead be approached from the perspective of personalized treatment that comprehensively considers patient age, menopausal timing, and overall health status. When treatment begins at the appropriate time, positive effects can be expected not only for quality of life improvement but also for long-term health management.”Q. How do you evaluate the FDA’s recent removal of the MHT Black Box Warning?Professor Tae-Hee Kim (Obstetrics and Gynecology, Soonchunhyang University Hospital Bucheon)Professor Tae-Hee Kim: I view this FDA action as an important opportunity to reevaluate the previously excessive perception of MHT risks based on evidence.The patients included in the WHI study had a median age of 63 and included women with cardiovascular risk factors. They differed from actual women in early menopause who typically begin hormone therapy. Moreover, the study used hormone combinations that are rarely used today, making it difficult to generalize the results to all patients.I think this decision carries significance in reorganizing overly emphasized risks so that women in early menopause who may benefit from hormone therapy do not avoid treatment excessively.”Professor Eun Sil Lee: The previous black box warning stated that prescribing MHT increased the risk of breast cancer, cardiovascular disease, and dementia, which significantly heightened patients’ fears. In fact, the frequency of hormone therapy use decreased significantly following the WHI study.However, subsequent age-specific analyses yielded different results. For women in their 50s who began treatment within 10 years of menopause, there was no clear increase in risk. On the contrary, the possibility of preventing cardiovascular disease or dementia was raised. Ultimately, this means that the timing of when hormone therapy is started is what matters.Q. How should the safety of MHT be evaluated?Professor Tae-Hee Kim: Previously, there was a strong perception that taking hormones increased the risk of cardiovascular disease and dementia, but in fact, these findings should be viewed as results from women who started treatment in their 60s and 70s.On the other hand, data is accumulating showing that starting treatment in one’s 50s, during the early stages of menopause, may actually have preventive effects against cardiovascular disease and dementia. Ultimately, the key issue is not simply whether or not to take hormones.Factors such as age, menopausal timing, and cardiovascular risk factors must all be considered comprehensively. I believe safety is determined by individualized treatment strategies tailored to each patient.Professor Eun Sil Lee: I believe the most important factors when evaluating safety are the patient’s age and the timing of menopause.In reality, women in the early stages of menopause often do not have a relatively high risk of cardiovascular disease. Rather, during this period, as hormone levels drop sharply, vascular health deteriorates, and changes such as decreased bone density, sleep disorders, and feelings of depression begin to manifest in earnest.Conversely, if a patient has already progressed into her 60s with advanced atherosclerosis, the approach may differ. In advanced atherosclerosis, hormone therapy could potentially affect thrombosis risk. In the end, the key issue is who starts treatment and when.In actual clinical practice, many patients with severe menopausal symptoms hesitated to pursue treatment due to fears such as ‘Won’t this increase my dementia risk?’ or ‘Won’t this cause cardiovascular disease?’ But recently, the concept of individualized treatment considering age, risk level, and menopausal timing has become increasingly important.Ultimately, I believe the safety of MHT is not an issue that can be explained in a one-size-fits-all manner; it must be assessed by comprehensively considering the patient’s health status and the timing of treatment.Q. How are differences in safety between products distinguished in actual clinical practice?Professor Eun Sil Lee: The approach to hormone therapy fundamentally differs depending on whether the patient has a uterus. Women without a uterus can use estrogen-only therapy, but women with a uterus must use progesterone in combination to prevent endometrial cancer.The characteristics of treatment differ depending on which progesterone is used. Appropriate therapy inevitably varies according to patient age, symptoms, risk level, and preference.Professor Tae-Hee Kim: Rather than saying a specific product is absolutely better, it is more accurate to view each hormone therapy as having distinct characteristics.It is important to select the most suitable medication by considering the patient’s lifestyle, symptoms, and health status. Ultimately, individualized treatment through consultation with a specialist is key.Q. How do you evaluate the breast cancer risk associated with MHT prescriptions?Professor Eun Sil Lee (Obstetrics and Gynecology, Soonchunhyang University Seoul Hospital)Professor Eun Sil Lee: In reality, differences exist depending on the medication. European studies showed that combinations of estrogen and natural progesterone did not demonstrate a clear increase in breast cancer, while some synthetic progesterone combinations showed tendencies toward increased risk.However, even if long-term use carries some increased risk, the absolute risk itself is interpreted as not very large. Above all, regular screenings are crucial.Women receiving hormone therapy tend to undergo regular screenings more consistently, and management is possible through early detection. Ultimately, I think accurate explanations are needed so patients do not abandon treatment based solely on vague fear.Professor Tae-Hee Kim: Many women have a vague fear that taking hormone therapy will cause breast cancer. But actual data show that the issue is not that simple.Even in the WHI study, women without a uterus did not show an increase, but rather a tendency toward reduced breast cancer incidence. European studies also found differences in breast cancer risk according to progesterone type. Some medications showed no significant increase.Of course, it cannot be said that taking hormones absolutely prevents breast cancer. However, the important point is that breast cancer mortality did not increase. In fact, overall mortality was lower.Benefits such as improved quality of life, fracture prevention, and cardiovascular disease prevention must also be considered together. Individualized treatment based on family history and risk level is important.Q. How do you predict MHT prescriptions will change in the Korean market going forward?Professor Tae-Hee Kim: I believe changes in perception toward MHT will clearly emerge in Korea as well. In particular, as life expectancy increases, interest is continuing to grow not only in living longer, but in aging healthily—that is, in ‘well-aging’ and ‘anti-aging.’Women now live for more than 30 to 40 years after menopause. Ultimately, how healthily this period is managed has become extremely important. From that perspective, hormone therapy should be viewed not merely as symptom control for hot flashes or sleep disorders, but as part of a healthy lifespan management strategy.Most important is the timing of treatment initiation. Starting treatment within 10 years after menopause or before age 60 is absolutely advantageous. Diseases such as cardiovascular disease, dementia, and osteoporosis become difficult to reverse once they progress. Therefore, we must approach them from a preventive perspective, which requires starting management from the early stages of menopause.In actual clinical practice, many patients experience major declines in quality of life due to osteoporotic fractures, fall risk, sleep problems, and joint pain. Hormone therapy can help improve these issues as well.Professor Eun Sil Lee: I believe the current prescribing environment is likely to expand further. However, rather than simply increasing prescriptions across the board, “personalized treatment” tailored to each patient’s characteristics will become more important.After menopause, vascular health deteriorates rapidly due to a decrease in estrogen. Atherosclerosis begins to progress, and bone density also decreases rapidly. Therefore, in women in the early stages of menopause, hormone therapy can play a positive role in preventing osteoporosis and maintaining vascular health.Conversely, the approach may differ for older women in whom atherosclerosis has already progressed significantly. Ultimately, this means that the patient’s age, vascular condition, and the timing of menopause must all be taken into account.Recently, the FDA has also emphasized the need for an approach that takes age and the timing of menopause into account. In fact, the FDA has recommended starting treatment within 10 years of menopause or before the age of 60.Most importantly, patient perception itself must change. Until now, the perception that ‘hormone therapy is always dangerous’ has been too strong. But now patients are beginning to think about both quality of life and healthy lifespan.Going forward, rather than simply enduring menopausal symptoms, interest in how to maintain health after menopause is likely to increase further. In that process, it will become important for patients to consult sufficiently with medical professionals and choose treatments suited to themselves.
- Company
- Curocell begins commercialization process for Korea's first CAR-T
- by Cha, Ji-Hyun May 15, 2026 02:44pm
- Curocell is pursuing market entry following the approval of South Korea's first domestically developed chimeric antigen receptor T-cell (CAR-T) therapy. Based on its domestic R&D and manufacturing infrastructure, the company aims to improve patient access to the CAR-T treatment landscape that has previously relied mostly on overseas facilities. Furthermore, the company plans to strengthen its next-generation pipeline through a strategy of expanding indications.On May 14, Curocell held a press conference at the Four Seasons Hotel in Seoul to commemorate the approval of its CAR-T therapy, 'Rimqarto Inj' (ingredient name: anbalcabtagene autoleucel). The company unveiled Rimqarto's clinical value, domestic commercialization strategy, and directions for subsequent clinical development. The event was attended by Curocell CEO Gunsoo Kim, Professor Won Seog Kim of Hemato-oncology at Samsung Medical Center, Curocell Executive Director Seungwon Lee, and Su-hee Cho, Head of Curocell’s Clinical Development Center.Rimqarto is an autologous CD19-targeting CAR-T therapy that uses a patient's own T cells. The process involves collecting T-cells from the patient's blood, introducing genes that allow them to recognize cancer cells, proliferating them ex vivo, and reintroducing them into the patient. It has been designed with Curocell's proprietary OVIS platform, designed to maximize therapeutic effects by simultaneously suppressing the expression of PD-1 and TIGIT, immune checkpoint receptors that inhibit the anticancer activity of T cells.Previously, on April 29, the Ministry of Food and Drug Safety (MFDS) granted marketing authorization for Rimqarto as a treatment for adult patients with relapsed or refractory diffuse large B-cell lymphoma (DLBCL) and primary mediastinal large B-cell lymphoma (PMBCL) after two or more lines of systemic therapy. With this, Rimqarto has been listed as the 42nd novel drug developed in Korea and the first CAR-T therapy developed by a Korean company.Curocell CEO Gunsoo KimCEO Kim shared in his opening remark that "The approval of Rimqarto is more than just one new drug entering the market. Curocell has step-by-step built a foundation that allows the entire process(from R&D to clinical trials, production, quality control, and licensing) to be performed domestically."CEO Kim emphasized that Rimqarto is a treatment option that can expand patient access in the CAR-T treatment landscape, which has been highly dependent on overseas supply. "For patients with relapsed or refractory DLBCL, treatment options are limited and disease progression can be rapid, making timely treatment critical," and added, "While existing CAR-T therapies faced barriers before reaching Korean patients in clinical settings, we will do our best to improve treatment accessibility and establish a stable supply base through Rimqarto."Professor Won Seog Kim, the first presenter, explained the unmet needs in DLBCL treatment and the clinical value of Rimqarto. According to Professor Kim, approximately 6,000-6,500 cases of malignant lymphoma occur annually in Korea, with DLBCL being the representative disease, accounting for 40% of cases. However, 35–40% of DLBCL patients experience recurrence after standard treatment, and patients reaching the third-line treatment stage number around 700 annually in Korea, carrying a poor prognosis.CAR-T therapies are considered an option that has changed the treatment paradigm in this relapsed/refractory DLBCL field. Professor Kim said, "In a patient group where the possibility of long-term survival was previously around 10%, data showed that CAR-T treatment could offer another treatment opportunity. For this reason, we could proceed quickly to obtain reimbursement, and added, "However, even with current commercial CAR-T therapies, the expectation for a complete cure remains at about 40%, leaving room for further improvement."Professor Kim presented Curocell's proprietary OVIS technology as Rimqarto’s distinguishment. One reason existing CAR-T therapies fail is that T-cells become exhausted or immune checkpoint mechanisms such as PD-1 or TIGIT become active, preventing the sufficient elimination of cancer cells."Curocell’s OVIS technology works by loading small RNA fragments into the CAR-T to suppress the expression of immune checkpoints like PD-1 and TIGIT," Professor Kim explained, "Rimqarto is a differentiated, next-generation CAR-T product in that it can overcome treatment failure caused byover-expression of immune checkpoints."On May 14, Curocell held a press conference to commemorate the approval of its CAR-T therapy, 'Rimqarto Inj' Clinical data also confirms Rimqarto’s competitiveness. In Phase 2 trial, Rimqarto demonstrated an objective response rate (ORR) of 75% and a complete response (CR) rate of 67% based on independent review committee evaluations. Regarding safety, the incidence of Grade 3 or higher cytokine release syndrome (CRS) was 9%, and neurotoxicity was 4%. Professor Kim said, "The response rate of over 75% and a CR rate of 67% as evaluated by the committee are highly encouraging results. It showed data that is manageable not only in terms of efficacy but also safety."Starting with this approval, Curocell plans to accelerate the commercialization of Rimqarto. Related to the core pillars of the commercialization strategy, Executive Director Lee Seung-won presented ▲rapid insurance reimbursement listing ▲expanding patient accessibility. "As CAR-T therapies are perceived as high-priced treatments, the speed of reimbursement listing is directly linked to patient access," Lee explained, " Rimqarto was selected for the parallel 'Approval-Evaluation-Negotiation' pilot project, listed on a track that can shorten the time from approval to reimbursement by approximately 90 days." Curocell is currently responding to supplementary data requests for the drug reimbursement evaluation and designing price-negotiation scenarios to support a reimbursed launch as early as September.The company will also pursue its domestic production base to build a supply chain and expand patient access. Lee stated, "Existing global CAR-T therapies involve a structure where a Korean patient’s cells are sent to an overseas manufacturing site and then brought back, which takes weeks and carries international transport risks. Rimqarto can achieve a fast 'vein-to-vein' time based on its domestic production facility." Curocell plans to establish a system within the year allowing Rimqarto treatment at 30 hospitals nationwide and will manage the entire process (from ordering to collection, manufacturing, delivery, and administration) through its online tracking platform, 'CuroLink.'On May 14, Curocell held a press conference to commemorate the approval of its CAR-T therapy, 'Rimqarto Inj' The company is also strengthening its next-generation pipeline by expanding Rimqarto's indications. As a follow-up development strategy, Curocell is considering expanding indications to adult acute lymphoblastic leukemia (ALL), systemic lupus erythematosus (SLE), and second-line treatment for DLBCL. Director Cho Su-hee explained, "There are currently no clear treatment options after standard therapy for patients over the age of 25, who make up the majority of adult ALL patients," and added, "Curocell has been preparing to expand the indication to adult ALL since 2022 and is currently in the final stages of Phase 1." The company plans to enter Phase 2 shortly and is also pursuing an expansion of clinical trials in Japan to strengthen global capabilities.The company is also pursuing expansion into autoimmune diseases and earlier lines of treatment. Director Cho stated, "To provide a better life for patients with lupus nephritis, we have started Korea's first autoimmune disease CAR-T clinical trial. Based on the experience of administering Rimqarto to lupus nephritis patients through "approval for use for therapeutic purposes," we expect encouraging results," and added, "Since Rimqarto showed a high response rate compared to other agents in third-line DLBCL, moving it up to second-line treatment would help even more patients."
- Policy
- Merck’s two new rare disease drugs receive GIFT designation
- by Lee, Tak-Sun May 15, 2026 02:44pm
- AI-generated imageThe Ministry of Food and Drug Safety (MFDS) is speeding up domestic approval timelines by designating two rare disease treatments from Merck as subjects for Korea’s Global Innovative products on Fast Track (GIFT) program.The MFDS announced that it designated Merck’s desmoid tumor treatment ‘Ogsiveo Tab’ and tenosynovial giant cell tumor (TGCT) treatment ‘Pimicotinib Cap’ as the 70th and 71st GIFT products, respectively. This designation is a measure to support the expedited approval of new drugs from innovative pharmaceutical companies that either have no existing treatment options or have demonstrated improved efficacy and safety.Ogsiveo Tab (nirogacestat hydrobromide), which was designated as a GIFT product on April 21, is a treatment for adult patients with desmoid tumors requiring systemic therapy. The drug suppresses tumor growth by inhibiting gamma secretase (GS) and blocking Notch signaling pathways.The drug has already received approval from the US FDA (November 2023) and the European EMA (August 2025), and was designated as an orphan drug in Korea on February 24, 2026. The MFDS selected it for expedited review based on the lack of existing treatment options.Then, on April 27, “Pimicotinib Cap (pimicotinib hydrochloride monohydrate),” a treatment for tenosynovial giant cell tumor(TGCT), was added to the GIFT list. The treatment works by selectively inhibiting the colony-stimulating factor-1 receptor (CSF-1R) to block disease progression.Pimicotinib is currently under development with FDA Fast Track and Breakthrough Therapy Designation (BTD) status in the United States, but has not yet received full approval in any global market. MFDS acknowledged the drug’s potential efficacy improvements and decided to manage it as a fast-track review product.The two products designated under GIFT will benefit from review periods shortened by approximately 25% compared to standard reviews. In addition, a rolling review of prepared materials and customized consultations with professional reviewers prior to the submission of the marketing authorization application will be provided, which is expected to significantly accelerate the timeline for the drug’s introduction in Korea.An MFDS official stated, “The exact indications and efficacy will be finalized after reviewing the submitted data. We will spare no effort in the review process to ensure that patients with intractable rare diseases can be provided with new treatment opportunities as quickly as possible.”
- Company
- GC Biopharma signs biopharma manufacturing MOU with Merck
- by Choi Da Eun May 15, 2026 02:43pm
- GC Biopharma is joining hands with global science and technology company Merck Life Science to strengthen its competitiveness in biopharmaceutical manufacturing. Through the partnership, the companies aim to secure stable supplies of key raw and subsidiary materials while improving manufacturing process efficiency to strengthen global market responsiveness.GC Biopharma announced on the 14th that it signed a strategic memorandum of understanding (MOU) with Merck Life Science for cooperation in biopharmaceutical development and GMP manufacturing processes.The signing ceremony was held at Merck Korea headquarters in Gangnam, Seoul. Major officials from both companies attended, including Young-im Kim, head of Merck Life Science Process Solutions Business, and Woong Shin, head of Quality Management at GC Biopharma.Through this agreement, GC Biopharma plans to strengthen cooperation on the supply of major raw and subsidiary materials needed for biopharmaceutical production and establish a collaborative framework to improve manufacturing efficiency and supply stability.In particular, GC Biopharma expects to secure a stable production base for major global products, such as its plasma-derived therapy Alyglo and the Hunter syndrome treatment Hunterase, both launched in the U.S. market, and respond more flexibly to changes in global demand.Merck plans to provide a collaborative framework covering the entire production process, from raw material procurement to process technology support. In particular, the companies aim to proactively manage supply chain risks that may arise during the manufacturing process by stably supplying product batches that meet strict internal quality control standards.The two companies also plan to operate a regular technical and process consultation body to strengthen technical cooperation for manufacturing process efficiency. Through this, they intend to share the latest production technologies and process know-how to enhance quality competitiveness, while continuously seeking joint R&D opportunities to expand their cooperative relationship.Woong Shin, Head of Quality Management at GC Biopharma, stated, “Through close technical cooperation and process optimization, we will work to minimize risks across the entire manufacturing process and build a production system with global-level quality competitiveness.”Young-im Kim, head of Merck Life Science Process Solutions Business, said, “Through this collaboration, we will work to support an optimal manufacturing environment so that GC Biopharma’s key therapeutic products can be supplied stably.”
- Company
- Rinvoq surpasses ₩100B in quarterly prescriptions
- by Kim, Jin-Gu May 15, 2026 02:43pm
- Product photo of Rinvoq Extended-release tabletAbbVie’s Janus kinase (JAK) inhibitor autoimmune disease treatment, ‘Rinvoq (upadacitinib),’ has strengthened its leading position by surpassing KRW 10 billion in quarterly prescriptions. Competing products such as ‘Olumiant (baricitinib),’ ‘Xeljanz (tofacitinib),’ and ‘Cibinqo (abrocitinib)’ showed sluggish performance.The JAK inhibitor market is expected to face even fiercer competition. This is due to the addition of new products such as Pfizer’s ‘Litfulo (ritlecitinib)’ and LEO Pharma’s ‘Anzupgo Cream (delgocitinib),’ as well as the launch of generics following the expiration of Xeljanz’s substance patent late last year.Rinvoq strengthens monopoly in JAK inhibitor market through expanded indicationsAccording to the pharmaceutical market research firm UBIST, on the 13th, Rinvoq's outpatient prescription volume in the first quarter was KRW 10.4 billion. This is a 32% increase compared to the KRW 7.8 billion recorded in the first quarter of last year. This marks the first time Rinvoq’s quarterly prescription performance has exceeded KRW 10 billion.Rinvoq received domestic approval in June 2020. Among JAK inhibitors, it was released third following Xeljanz and Olumiant, but it rapidly expanded its influence. Since the fourth quarter of 2023, Rinvoq has risen to the top of the market. Since then, it has been strengthening its monopoly by widening the gap with competing products.In contrast, Rinvoq’s major competitors appear sluggish. Olumiant, the second-ranked product in the market, recorded KRW 4.5 billion in first-quarter prescriptions, a slight decrease compared to KRW 4.6 billion in the first quarter of last year.During the same period, Xeljanz decreased by 21% from KRW 3.5 billion to KRW 2.8 billion KRW. This was influenced by a price reduction following the listing of generics for reimbursement in November last year. The prices of two dosages of Xeljanz tablets were cut by 30%, while the price of Xeljanz XR extended-release tablets was reduced by 23%. ‘Cibinqo,’ which Pfizer launched as a successor to Xeljanz, decreased from KRW 1.6 billion to KRW 1.5 billion.Jyseleca, which entered the market as the fifth JAK inhibitor, is significantly improving its prescribing performance. In the first quarter of this year, it recorded KRW 1.8 billion in prescriptions, a 2.6-fold increase compared to the same period last year.Prescription volume changes for major JAK inhibitors (unit: KRW 100 million, source: UBIST). GREEN-Rinvoq, PINK-Olumiant, BLUE- Xeljanz, LIGHT GREEN- Jyseleca, PURPLE- CibinqoThe aggressive strategy of expanding indications is cited as the background for Rinvoq’s strengthened dominance. Currently, Rinvoq holds six indications ▲rheumatoid arthritis ▲psoriatic arthritis ▲axial spondyloarthritis (ankylosing spondylitis) ▲atopic dermatitis (adults and adolescents) ▲ulcerative colitis ▲Crohn’s disease. It has secured the most indications among JAK inhibitors.In addition, AbbVie recently succeeded in global Phase 3 clinical trials for alopecia areata, signaling the addition of a seventh indication. Besides alopecia areata, AbbVie is also pursuing expansions into subsequent immune disease indications such as vitiligo, hidradenitis suppurativa, systemic lupus erythematosus, and Takayasu arteritis.Its competitor, Xeljanz, has five indications ▲rheumatoid arthritis ▲psoriatic arthritis ▲ankylosing spondylitis ▲ulcerative colitis ▲polyarticular juvenile idiopathic arthritis ▲juvenile psoriatic arthritis. Olumiant holds four indications ▲rheumatoid arthritis ▲atopic dermatitis (adults and children) ▲alopecia areata (adults) ▲juvenile idiopathic arthritis. Cibinqo has only atopic dermatitis (adults and adolescents) as an indication, while Jyseleca has indications for rheumatoid arthritis and ulcerative colitis.Emergence of 6th and 7th JAK inhibitors and Xeljanz generics late last yearFiercer competition in this market is expected in the future with the addition of the sixth and seventh new JAK inhibitor drugs and Xeljanz generics.Recently, ‘Litfulo’ was launched as the sixth JAK inhibitor. This product received domestic approval in September 2024 and was released as a non-reimbursed drug in February of last year. Its indication is alopecia areata in adults and adolescents aged 12 and older. Pfizer now possesses three JAK inhibitors: Xeljanz, Cibinqo, and Litfulo.In September last year, LEO Pharma received approval for ‘Anzupgo Cream,’ the first topical JAK inhibitor in Korea, for the treatment of chronic hand eczema. LEO Pharma officially launched this product in March of this year. It is currently non-reimbursed.In November last year, a large number of generics containing the ingredient tofacitinib entered the market due to the expiration of the Xeljanz patent.A total of 59 companies have received approval for Xeljanz generics, and products from 14 companies, including Daewoong Pharmaceutical, Il-Yang Pharmaceutical, and Chong Kun Dang, are currently listed on the reimbursement list. However, the prescription volume remains still.
- Company
- MSA left unmanaged despite being a rare neurological disorder
- by Son, Hyung Min May 15, 2026 02:43pm
- Concerns are being raised that multiple system atrophy (MSA), a fatal neurodegenerative disease characterized by faster progression and a heavier disability burden than Parkinson’s disease, still remains outside an independent rare disease management framework in Korea.Unlike major overseas countries that operate separate registration and support systems, Korea still lacks even an accurate understanding of the patient population due to mixed disease coding and limited support measures.At the recent “Denmark-Korea Roundtable on MSA Care” held at the Embassy of Denmark in Korea, domestic and international experts discussed the clinical characteristics of MSA, diagnostic limitations, gaps in long-term care, and the need for rare disease designation. Experts on movement disorders from both Korea and Denmark attended the event to share their management systems.“Denmark-Korea Roundtable on MSA Care” event hosted by the Danish Embassy in Korea.Mikael Hemniti Winther, Ambassador of Denmark to Korea, said in his welcoming remarks, “Patients with rare and intractable neurological diseases require not only access to treatment but also long-term care and social support systems. “I look forward to Denmark and Korea sharing clinical experiences and policy models to further develop patient-focused care systems.”MSA is a progressive neurodegenerative disease in which multiple parts of the nervous system, including the basal ganglia, cerebellum, and brainstem, atrophy simultaneously. While it begins with symptoms similar to Parkinson’s disease, such as stiffness and slowed movement, as the disease progresses, autonomic nervous system abnormalities rapidly develop, including orthostatic hypotension, urinary dysfunction, sleep disorders, and respiratory difficulties.As a result, the disease shows limited response to levodopa-based therapies commonly used for Parkinson’s disease, while symptom progression is significantly faster. According to existing data, the average survival period for MSA patients is known to be approximately 6 to 10 years after symptom onset, and it is not uncommon for patients to require walking aids or wheelchairs within a few years of diagnosis.Professor Do-Young Kwon of the Department of Neurology at Korea University Ansan Hospital said, “Although MSA is rare enough to be classified as a rare disease, its clinical and social impact is extremely severe. MSA patients suffer not only from Parkinsonian symptoms but also cerebellar ataxia, autonomic dysfunction, and sleep disorders, and many progress to severe disability within a few years.”Currently, Korean healthcare big data estimates the number of MSA patients at fewer than 3,000 as of 2024. However, in actual clinical practice, many cases are reportedly registered and managed under the Parkinson’s disease code (G20). Academia views this code overlap as one of the major reasons why the true patient population and disease burden are not properly reflected.There are also significant differences in MSA management compared with other countries. The United States operates incentives for MSA drug development under the Orphan Drug Act, while Japan has established patient registration and medical expense support systems through its designated intractable disease framework. Europe likewise operates national-level management systems based on rare disease coding and research networks.In contrast, Korea does not manage MSA within a separate rare disease framework, leading to insufficient support systems tailored to the disease’s characteristics, including long-term rehabilitation, palliative care, and sleep and respiratory management.Rapid progression and complex symptoms…limits of treating MSA the same as Parkinson’s diseaseProfessor Sooyeon Yoo, Seoul Medical Center, Department of NeurologyProfessor Sooyeon Yoo of the Department of Neurology at Seoul Medical Center emphasized that diagnosing MSA itself is not easy.Professor Yoo explained, “MSA often presents symptoms very similar to Parkinson’s disease in the early stages. In some patients, characteristic autonomic nervous system abnormalities or imaging changes only appear after specific symptoms have progressed, so delayed diagnosis is common.”In clinical practice, it reportedly takes an average of 3-4 years to reach an accurate diagnosis. The problem is that during this period, patients may remain in a treatment gap without appropriate rehabilitation or long-term care planning.Professor Yoo said, “MSA patients experience severe declines in quality of life due to sudden fainting, falls, urinary dysfunction, and impaired temperature regulation. It places a significant psychological and financial burden not only on patients but also on their caregivers.”She added, “Since there is currently no fundamental treatment capable of slowing disease progression, it is important to establish support systems that integrate rehabilitation, respiratory care, sleep management, and palliative care over the long term. We need a structure within the public healthcare system that ensures patients receive continuous care.”Professor Jinyoung Youn of the Department of Neurology at Samsung Medical Center also pointed out the limitations of the current system, which manages MSA at the same level as Parkinson’s disease.Professor Jinyoung Youn, Department of Neurology, Samsung Medical Center“Many Parkinson’s disease patients are able to maintain daily life for long periods through medication management, MSA involves a much more rapid decline in physical function. There are currently no medications available to improve cerebellar symptoms.”He further explained that because MSA presents with a complex combination of symptoms, a single-department approach has clear limitations. In fact, some medications may alleviate Parkinson’s symptoms but exacerbate others, such as orthostatic hypotension or constipation.Professor Youn said, “It is common for drugs used to control one symptom to aggravate another. A multidisciplinary approach involving not only neurology but also urology, pulmonology, rehabilitation medicine, and sleep medicine is essential.”In particular, he pointed out that a significant portion of the rehabilitation, sleep therapy, respiratory support, and long-term care services required by MSA patients are still not adequately covered under the current system.Professor Youn noted, “MSA patients often develop the disease at relatively younger ages and tend to preserve cognitive function comparatively well. As a result, many do not fit well within existing long-term care facilities or dementia-centered caregiving systems.”The Danish case stood in contrast to Korea’s current reality.Professor Anne-Mette Hejl of Bispebjerg-Frederiksberg Hospital in Denmark stated, “In Denmark, neurologists, specialized nurses, physical and occupational therapists, and neuropsychology experts collaboratively manage MSA patients. Depending on the patient’s condition, services are linked to telemedicine, home care, and hospice care.”“Denmark-Korea Roundtable on MSA Care” event hosted by the Danish Embassy in Korea.In practice, Denmark operates a system that reduces caregiving burdens for patients and families through follow-up observations every 3 months, extended consultations, and connections to home-based services. When hospital visits become difficult, patients are transitioned to telemedicine and community-based care systems.To date, there are no treatments available that can fundamentally slow or halt the progression of MSA itself. Consequently, experts generally agree that the importance of early diagnosis, rehabilitation, respiratory and sleep management, and long-term care systems is becoming increasingly prominent.Meanwhile, global pharmaceutical companies continue to develop therapies aimed at suppressing MSA progression. Lundbeck’s “Amlenetug” has entered global phase 3 clinical trials, while Teva’s “Emrusolmin,” BioArctic’s “Exidavnemab,” and Alterity Therapeutics’ “ATH434” are also in clinical development stages.Experts believe that if disease-modifying therapies become available in the future, the importance of early diagnosis and national patient registration systems will grow even further.