- LOGIN
- MemberShip
- 2026-05-03 23:15:17
- Policy
- Takeda's drug pricing negotiations see different results
- by Lee, Tak-Sun Sep 25, 2024 05:48am
- The drug pricing negotiations for ‘Ceprotin (Protein C Concentrate (Human))’ a new drug for severe congenital protein C deficiency supplied by Takeda Pharmaceuticals Korea, fell through. On the other hand, the company reached an agreement and completed negotiations to expand the reimbursement for the ovarian cancer treatment Zejula Cap. According to industry sources on the 24th, the National Health Insurance Service announced so while updating the list of drugs that have completed drug price negotiations. Ceprotin passed the NHIS’s Drug Reimbursement Evaluation Committee in June and began negotiating with the NHIS in July, which is the final step to a drug’s reimbursement in Korea. The drug was first approved in Korea in 2022 for the treatment of severe congenital protein C deficiency. Congenital protein C deficiency is a rare genetic condition that causes a fatal defect in the regulation of blood clotting due to a lack of protein C. It affects 1 in 4 million newborns. As the only treatment available, patients have been longing for its reimbursement, but the opportunity has passed this time. Therefore, it remains to be seen whether Takeda will reattempt its reimbursement in the future. Meanwhile, reimbursement for Takeda's Zejula Cap, which passed DREC review along with Ceprotin, will be expanded in October with the finalization of negotiations. Zejula is currently reimbursed for patients with BRCA mutations as maintenance therapy in the first- to second-line treatment of platinum-sensitive advanced ovarian cancer who have responded to platinum-based chemotherapy. In October, the reimbursement standards will change from ‘patients with BRCA mutations’ to ‘patients who are Homologous Recombination Deficiency (HRD) positive.’
- Company
- Cancer mRNA vaccine shows potential in brain tumor
- by Son, Hyung Min Sep 24, 2024 05:46am
- Therapeutic cancer vaccines have been showing promise in central nervous system diseases. CureVac recently confirmed the safety of its messenger ribonucleic acid (mRNA) vaccine, CVGBM, in glioblastoma in a Phase I clinical trial. Immunomic Therapeutics and IM Biologics have also taken up the challenge of developing cancer vaccines for brain tumors. Cancer vaccines are therapeutic vaccines that treat cancer by administering cancer cell antigens to patients and activating the immune system rather than prevention vaccines. Like conventional vaccines, cancer vaccines also work with the same mechanism of action, activating the body’s immune response and inducing immunogenic cell death. Major pharmaceutical and biotech companies are focusing on maximizing the treatment effect rather than prevention, and are using strategies to increase their vaccine’s commercialization potential by combining its use with anticancer drugs. Cancer vaccines with various mechanisms of action are being developed...targets brain tumors According to industry sources on the 23rd, Germany's CureVac recently unveiled the first-in-human trial results of its mRNA cancer vaccine candidate 'CVGBM' in treating glioblastoma. Glioblastoma is a type of glioma, a malignant tumor that occurs primarily in the brain. Glioblastoma has a poor prognosis, with a 5-year survival rate of a mere 5% despite surgery and chemoradiotherapy. The average survival time is only about one year. CureVac’s CVGBM is an investigational therapeutic mRNA-based vaccine encoding 8 epitopes derived from tumor-associated antigens with potential relevance in glioblastoma. An mRNA cancer vaccine constructs abnormal proteins (neoantigens) produced by cancer cells. The body's immune cells then produce antibodies to respond to them, which then kills cancer cells. CureVac is currently conducting a Phase I trial in MGMT-unmethylated glioblastoma, which is known to have a poor prognosis. As of February 29, 2024, 16 patients with glioblastoma have been enrolled in the trial. The primary endpoints were safety, tolerability, and dose-limiting toxicities (DLTs) in CVGBM. Immunogenicity was included as an exploratory endpoint. Clinical results showed that the most common treatment-emergent adverse events (TEAEs) were chills (13 patients), fever (12 patients), headache (12 patients), and fatigue (11 patients). Most patients experienced mild-to-moderate symptoms. “CVGBM was generally well tolerated with an acceptable safety profile,” the researchers concluded. ”Based on all available safety data, the dose selected for clinical expansion was 100 μg. Patients did not reach the maximum tolerated dose.” CureVac is continuing to monitor clinical progress and plans to present the first immunogenicity data once results are confirmed. Meanwhile, a U.S. company, Immunomic Therapeutics has completed a Phase II clinical trial of its glioblastoma cancer vaccine, ITI-1000. ITI-1000 is a cancer vaccine based on Immunomic's cell therapy vaccine platform (UNITE) that activates “dendritic cells,” the immune system's watchdogs, to kill tumors. ITI-1000 activates dendritic cells to recognize the ‘pp65′ protein of cytomegalovirus, which is present in glioblastoma and alerts other key immune cells when a pathogen invades the body. Currently, Immunomic has completed its Phase II clinical trial and is in the process of analyzing the data. Published clinical results to date have shown that ITI-1000’s median overall survival (OS) is over 30 months. Companies in Korea are also developing cancer vaccines targeting brain tumors. IM Biologics' glioblastoma cancer vaccine candidate 'IMB-402' was selected as a new project of the Ministry of Trade, Industry and Energy's ‘Material Parts Technology Development Project.’ IMB-402 is a cancer vaccine candidate that selectively proliferates and activates glioblastoma (GBM)-specific T cells by applying an ampeptide-HLA complex to ePENDY, an IgM antibody-based multimer platform. IM Biologics designed IMB-402 with additional co-stimulatory factors to prevent activated T cells from falling into a lethargic state. IMB-402 is currently in the candidate optimization phase, and the company plans to secure the candidate and conduct non-clinical studies through this project.
- Company
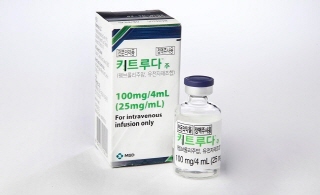
- 'Keytruda' attempts at reimbursement for TNBC
- by Whang, byung-woo Sep 24, 2024 05:46am
- The industry watches whether Keytruda (pembrolizumab), which demonstrated treatment benefits in early triple-negative breast cancer, will pass the reimbursement hurdle. As the Cancer Disease Review Committee (CDRC) of the Health Insurance Review and Assessment Service (HIRA) convenes in October, whether Keytruda will set a ground to expand 17 indications will be watched. Product photo of KeytrudaAccording to the pharmaceutical industry, the HIRA will convene the 7th Cancer Disease Review Committee (CDRC) meeting on October 2nd. Currently, Imfinzi (durvalumab) and Jemperli (dostarlimab) are applying for reimbursement expansion. The review of Keytruda, which has applied for reimbursement of 17 indications, is garnering attention. In April, the CDRC review postponed setting the criteria for Keytruda, saying, 'We will reconsider setting the reimbursement criteria when the company submits a supplement for financial contribution.' While many indications seek reimbursement listing, tiple-negative breast cancer outcome is gaining attention. MSD presented the KEYNOTE-522 study, which confirmed the overall survival (OS) data for Keytruda in high-risk early triple-negative breast cancer, during the recent European Society for Medical Oncology (ESMO) Congress 2024. The KEYNOTE-522 study is a Phase 3 clinical trial evaluating Keytruda in combination with cancer chemotherapy as a perioperative adjuvant therapy. During the median 75.1 months follow-up, Keytruda perioperative adjuvant therapy in patients with high-risk early triple-negative breast cancer significantly improved the OS compared to the placebo group. Sohn, Joo Hyuk, Professor of the Division of Oncology at Yonsei Cancer Hospital, said, "In early cancer treatment aiming for complete recovery, it is not easy to demonstrate improvement in the OS rate. Improving the OS rate is a meaningful result in that it indicates saving lives of patients with early triple-negative breast cancer." The experts suggest that since the study results demonstrate clinical data to be considered for reimbursement evaluation, it may be sufficient to prove its effectiveness. Park Yeon Hee, Professor of the Department of Hematology-Oncology at Samsung Medical Center, said, "With data demonstrating improvement in OS rate, it must be considered for reimbursement review," adding, "Because patients with triple-negative breast cancer are young and economically active, the drug's societal value must be considered as well." Park added, "For patients, a diagnosis of triple-negative breast cancer diagnosis may have felt like a disaster. Keytruda offers hope to these patients. It is meaningful that early intervention may eliminate the need for follow-up treatment." The problem will likely be the cost. Because the CDRC review in April stated, 'We will reconsider setting the reimbursement criteria when the company submits a supplement for a financial contribution,' the company may need to make more financial contribution. However, the experts suggest that reimbursement for the drug may be possible for use in combination with perioperative chemotherapy, where the volume of use at 8 cycles is predictable, when considering its impact on the National Insurance finance. As the company applies for reimbursement of Keytruda's 17 indications, approval outcome by individual indication is not easily determined. Whether Keytruda's triple-negative breast cancer indication will pass the reimbursement hurdle is not clear. An industry personnel said, "Keytruda's reimbursement application, including the individual indication with few patients, has drawn attention, but the company is discussing other strategies after not passing the CDRC review," adding, "The company will likely think over the strategy after the upcoming CDRC review now that it has more indications than the initial 13."
- Company
- Samsung Bioepis’ Opuviz recommended for approval in Europe
- by Whang, byung-woo Sep 24, 2024 05:46am
- Pic of Samsung Bioepis office building Samsung Bioepis announced on the 23rd that the European Medicines Agency’s (EMA) Committee for Medicinal Products for Human Use (CHMP) has adopted a positive opinion for the company’s Eylea biosimilar ‘Opuviz (aflibercept).’ The EMA CHMP’s positive opinion plays a crucial role in the marketing authorization review process by the European Commission (EC), whose results typically follow 2-3 months after receipt of the positive opinion. Eylea, Opuviz’s original version, is a treatment for eye diseases such as wet age-related macular degeneration developed by the U.S. company Regeneron. The drug binds to vascular endothelial growth factor (VEGF) and inhibits neovascularization. It has annual global sales of approximately KRW 12 trillion. Macular degeneration is a disease that impairs vision due to aging and inflammation of the macula, the nerve tissue located in the center of the retina. The condition can cause blindness in severe cases and requires continuous treatment to slow the progression. Samsung Bioepis has launched a total of 8 biosimilar products in the European market. If approved, Opuviz is expected to expand the company’s portfolio of ophthalmology treatments in the European market, following the company’s existing eye disease treatment, Byooviz (Lucentis biosimilar, ranibizumab). “We are pleased to have our second ophthalmology biosimilar Opuviz recommended for approval in Europe,” said Byoungin Jung, Vice President and Regulatory Affairs Team Leader at Samsung Bioepis. “We will continue our efforts to provide patients with more treatment options by continuing to advance our broad pipeline.” Meanwhile, Samsung Bioepis obtained approval for Opuviz in the U.S. in May and has been selling it in Korea under the brand name Afilivusince May through its partner, Samil Pharmaceutical.
- Policy
- Pharmbio releases first generic Revolade with reimb in OCT
- by Lee, Tak-Sun Sep 24, 2024 05:46am
- The first generic version of the immune thrombocytopenia treatment ‘Revolade (eltrombopag olamine)’ will be released into the market in October. Pharmbio Korea’s Revolade generic has succeeded in receiving reimbursement listing 1 year after its approval in Korea. The company had been delaying its launch due to the burden of patent infringement, but its recent success in avoiding the patent prompted it to launch the product in full force. According to industry sources on the 23rd, Pharmbio Korea’s Elpag Tab. 25 mg and 50 mg will be listed for reimbursement from October 1st. The items were approved in March last year. As a rare disease drug used for thrombopenia, Elpag Tab is a generic version of Novartis’s Revolade. Although Revolade's product patent has expired, 3 composition patents are listed on MFDS’s green list, making it difficult for latecomer generics to enter the market. Pharmbio Korea and SK Plasma sought to evade Revolade ‘s substance patent by filing for a passive trial to confirm the scope of the patent. The Intellectual Property Trial and Appeal Board ruled in favor of the generic companies’ claims in the first half of this year, clearing the patent hurdle. However, the patent dispute is not completely resolved as Novartis immediately filed a following suit to cancel the decision. In this situation, Pharmbio has decided to preemptively launch its product through reimbursement listing. Revolade treats immune thrombocytopenia (ITP), a type of bleeding disorder, by stimulating platelet production. ITP is an autoimmune disease in which the immune system mistakes the body’s platelets as foreign and attacks them. According to IQVIA, Revolade’s domestic sales amounted to KRW 9 billion last year. Pharmbio is challenging the original drug with a lower price. It has applied for a drug price lower than the calculated price, setting the price at KRW 22,849 for Elpag Tab 25 mg and KRW 44,405 for Elpag Tab 50 mg. This is 30% lower than the price of the original Revolade 25mg, which is priced at KRW 32,641, and Revolade 50mg at KRW 63,435. In the case of orphan drugs, the price is set at the same level as previously listed drugs. Pharmbio seems to have adopted a strategy to increase its market share through a relatively low price.
- Company
- Will Wegovy launch in KOR continue the Saxenda syndrome?
- by Moon, sung-ho Sep 24, 2024 05:46am
- 'Wegovy,' an obesity drug that is hugely popular but in shortages worldwide, will land in South Korea in mid-October. It will become domestically available a year and a half after receiving approval from the Ministry of Food and Drug Safety (MFDS). It marks the ninth release worldwide, following Japan and China. The Wegovy effect has garnered attention from university hospitals and private clinical practices in light of the news. The industry is watching whether the Wegovy sales will match those of the obesity drug 'syndrome' in the mid-2010s when Saxenda (liraglutide) was released in South Korea. Product photo of Wegovy.According to the pharmaceutical industry on September 23rd, Novo Nordisk Korea announced the launch of the obesity drug 'Wegovy Prefilled Pen (semaglutide)' in mid-October in South Korea. This detailed announcement of the product launch date may be due to increasing interest in the domestic introduction of the global obesity drugs, such as Wegovy. Wegovy is an obesity drug and a once-weekly injectable prescription drug. In early April 2023, the MFDS approved the use of Wegovy as a weight-loss and weight-management aid to obese patients who have a Body Mass Index (hereafter referred to as BMI) of 30kg/m2 or higher or those who are overweight with early BMI of 27kg/m2 or higher and below 30kg/m2 and having one or more weight-related accompanying diseases. Furthermore, Wegovy's expanded indication was approved for use in reducing the risk of major cardiovascular events (cardiovascular diseases-related deaths, non-critical myocardial infarction or non-critical stroke) in patients who have confirmed cardiovascular diseases and are overweight, or obese with a BMI of 27 kg/m2 or higher at an early stage. As South Korea has been set as the 10th country worldwide to have Wegovy launched, physicians have both hopes and concerns. The vast opinion is that Wegovy will gather more interest than Saxenda which may cause a 'syndrome.' The concern is that when the stock is supplied in a limited quantity, patients may attempt various illegal transactions to obtain the drug. Because it is being launched domestically to clinical practices as a non-reimbursable drug, Wegovy is expected to be primarily used by patients who want it for health management and beauty instead of those with clinical needs, such as overweight patients. Sung-Rae Kim, Chairman of Korean Society for the Study of Obestiy (KSSO) and Professor of the Catholic University of Korea Bucheon St. Mary's Hospital (Endocrinology), said, "It is great news that Wegovy will be launched in South Korea, world's 10th country. However, I am concerned whether it will be used properly because of the non-reimbursable status," adding, "For Ozempic, a diabetes drug containing the same active ingredient, it did not pass the hurdle of the reimbursement listing process after the domestic launch. Since new drugs cannot be introduced with reimbursement due to the current Korean drug pricing system, we need to think over this issue." Kim said, "When I reviewed the Korean obesity statistics, the obesity rate is higher in individuals who have socioeconomic difficulties. As the drug will not be covered by insurance, I am concerned whether it will be properly used for obesity treatment," and explained, "In my opinion, I hope that a specific stock will be utilized for treating patients with obesity, covered by insurance coverage." In the past few years, by Saxenda and Qsymia have dominated the Korean obesity market. This division is expected to disappear when Wegovy enters sales. In the meantime, private clinical practices are sharing opinions about Wegovy's expected non-reimbursement price after its launch. Although Novo Nordisk has yet to announce the price, clinical practices are hopeful that it will be the 'lowest price' worldwide as a non-reimbursable drug. In reference, Wegovy is sold in the United States for US$1,350 (around KRW 1.8 million) per month. This is about KRW 21.6 million for a year-long treatment. For Japan, the monthly treatment costs are set about KRW 400,000 with insurance coverage. Private clinical practices expect the price of Wegovy in South Korea to be the lowest in the world for a non-reimbursable drug, except for Japan's cases with insurance coverage. The clinical field suggests this is likely due to Mounjaro (tirzepatide, Lily Korea). Wegovy seems to be attempting to dominate the market by entering the domestic clinical field ahead of Mounjaro, which does not have a set launch date. Cost-wise, Mounjaro is sold at a cheaper price than Wegovy in the global market. Consequently, Wegovy might launch in South Korea before Mounjaro. A family medicine physician who remained anonymous said, "Wegovy in Japan appears to be the world's lowest price. However, it is covered by insurance. As a non-reimbursable drug, Wegovy is expected to launch in Korea at the lowest price," adding, "Novo Nordisk may be contemplating on a reasonable non-reimbursable price. Although the price has yet been set, the company may be considering Mounjaro's domestic launch." "A yearly treatment for Mounjaro is about KRW 3 million cheaper than Wegovy when converted, and the vial formulation is 50% lower in drug price," and analyzed, "Considering many points, the company is likely planning to enter the Korean market with Wegovy before Mounjaro." Korean clinical field expects that Wegovy will result in the new obesity drug syndrome, surpassing that of Saxenda, and cause major shifts in the industry, such as bringing changes to the medical system and healthcare. Doctor Chul-Jin Lee, President of DAOR, said, "Since patients are already familiar with obesity drugs because of Saxenda, so setting the right drug price will generate immediate interest, surpassing the syndrome," and explained, "Taking the Korean market into account, Wegovy is just the beginning. Other drugs with various formulations and Mounjaro will follow." Lee added, "Divisions in the Korean medical system are not divided, but diseases connect all divisions. There could be an increase in patients with digestive trouble when Wegovy launches in Korea," adding, "In the United States, the healthcare supplement industry has changed, with supplements becoming more available in pharmacies following the Wegovy launch. Similarly, the Korean medical system and related industry will likely undergo change."
- Company
- Severe asthma biologic 'Nucala' available in the 'Big 5'
- by Eo, Yun-Ho Sep 24, 2024 05:46am
- Product photo of GSK The biologic antibody drug 'Nucala' is now available for prescription at tertiary general hospitals. According to industry sources, GSK's Nucala (mepolizumab), a treatment for severe neutrophilic asthma, has passed the drug committees of the 'Big 5' tertiary hospitals, including Samsung Medical Center, Seoul University Hospital, Seoul Asan Medical Center, and Sinchon Severance Hospital, and Seoul St. Mary's Hospital. After being listed to the reimbursement list in November, this drug is becoming more widely available in hospitals. Nucala is an anti-interleukin (IL)-5 that reduces counts of neutrophils, a type of white blood cell contributing to asthma. It can be prescribed to ▲patients with neutrophil counts of 150 cells/㎕ or more at the start of treatment ▲adult patients with severe neutrophilic asthma who have neutrophil counts of 300 cells/㎕ or more within 12 months of treatment as an add-on maintenance therapy. The efficacy of Nucala has been demonstrated through the Phase 3 DREAM, MENSA, and SIRIUS studies. The MENSA study results were published in NEJM in 2014. The study involved patients with severe asthma who had worsened symptoms despite the previous use of several agents, such as high-dose inhaled corticosteroids (ICS). The investigators enrolled patients with neutrophil counts of 150 cells/㎕ or more (300 cells/㎕ or more a year before) at the time of the initial screening test. The patients were given mepolizumab or placebo, and they were monitored for annual rate of worsened symptoms. The results showed that patients administered an intravenous injection of mepolizumab 75 mg had a 47% reduction in the annual rate of worsened symptoms compared to the placebo group. The patients administered a subcutaneous injection of mepolizumab 100 mg had 53% reduction in the rate. Furthermore, the quality of life improved, and patients had higher satisfaction with asthma control than the placebo group. The SIRIUS study involved patients who use oral corticosteroids (OCS) and evaluated the changes in OCS dosage after 20-24 weeks of mepolizumab treatment. The study results showed that the mepolizumab 100 mg patient group had a 50% reduction in the OCS dose compared to the placebo group and significantly improved asthma control satisfaction and quality of life evaluation. The study was the first research to prove that an antibody drug can reduce OCS dosage. It was published in the European Respiratory Journal (ERJ) in 2014. Meanwhile, drugs with similar mechanisms to Nucala are Teva-Handok's 'Cinqair (reslizumab)' and AstraZeneca’s 'Fasenra (benralizumab).' Cinqair was listed to the reimbursement list at the same time as Nucala, and Fasenra was listed since July.
- Company
- Hugelsets sights on Indonesia with botulinum toxin Letybo
- by 어윤호 Sep 23, 2024 09:40am
- Hugel and its Indonesian partnerParvus host a launch event of botulinum toxin Letybo at Shangri-La JakartaHugel Inc., a leading global medical aesthetics company, said on Monday it had hosted a launch event of Letybo last week at Shangri-La Jakarta in Indonesia, the second-largest medical aesthetics market in Southeast Asia, to promote the clinical efficacy of the botulinum toxin. The event comprised online and on-site lectures on techniques and trends of Letybo treatment. The lectures were led by Dr. Konstantin Frank, a plastic surgery resident at Ocean Clinic, Marbella in Spain, and medical aesthetics industry leaders in Indonesia. Prior to the launch event, Hugel conducted a hands-on workshop on the safe and effective treatment of botulinum toxin for local doctors. Dr. Frank delivered an anatomy lecture on Letyboinjection for Asians and performed live demonstrations for around 350 healthcare and medical professionals. “We are pleased to have launched our premium botulinum toxin product Letybo in Indonesia, Southeast Asia’s second-largest medical aesthetics market after Thailand. Hugel will continue to engage with local practitioners through seminars and workshops for promotion ofLetybo’s prowess,” a Hugel official said.
- Company
- Why royalties for Yuhan’s Leclaza were reduced $300mil
- by Chon, Seung-Hyun Sep 23, 2024 05:51am
- The maximum contract amount for Leclaza, which was licensed out to Janssen by Yuhan Corp, has been reduced by USD 350 million. This reduction was due to the termination of research to develop Leclaza as a next-generation anti-cancer drug. Yuhan Corp received USD 210 million as upfront payment and development and approval milestones for the licensing agreement and is eligible to receive up to USD 740 million upon further development and sales. Pic of Yuhan Corp headquartersOn the 20th, Yuhan Corp publicly announced that the maximum deal for Leclaza’s technology transfer agreement with Janssen Biotech has been reduced by USD 350 million (KRW 406.5 billion) from USD 1.255 billion to USD 950 million. The company explained that the reduction was due to “partial corrections to the agreement due to the termination of collaborative research and development of next-generation (4th generation) EGFR (epidermal growth factor receptor) targeted anticancer therapy.” In November 2018, Yuhan Corp licensed out its anti-cancer drug Leclaza to Janssen Biotech. The total value of the agreement, including a non-refundable upfront payment of USD 50 million, amounted to USD 1.25 billion. The term of the agreement is from the date of the agreement until the expiration of the country-specific patent rights or 12 years from the date of the first commercial sale in each country, whichever comes later. The technology transfer agreement also included rights to develop a fourth-generation EGFR tyrosine kinase inhibitor (TKI). Third-generation EGFR TKIs were primarily developed for the treatment of NSCLC with EGFR gene mutations, most notably the T790M mutation. The T790M mutation occurs in patients who show resistance to existing first- and second-generation EGFR TKIs. According to the company, 4th generation EGFR TKIs target a broader genetic mutation profile than existing EGFR TKIs as they selectively inhibit key mutations that lead to resistance to 1st to 3rd generation EGFR TKIs. Janssen had studied the combination of the 3rd generation EGFR-targeted cancer drug Leclaza and Johnson & Johnson's bispecific antibody amivantamab. Janssen successfully completed the clinical trial for Leclaza in combination with amivantamab and received U.S. Food and Drug Administration (FDA) approval last month for the combination of Leclaza and Rybrevant as a first-line treatment for adult patients with locally advanced or metastatic NSCLC who have a confirmed EGFR exon 19 deletion or exon 21 L858R substitution mutation. “The significant reduction in the incidence of secondary resistant EGFR mutations in patients treated with the Leclaza and amivantamab combination reduces the need for further development of a 4th generation EGFR TKI,” the company said. In other words, the company explained the combination of Leclaza and amivantamab has been so effective that it has ended attempts to develop a next-generation drug. Yuhan has received a total of USD 210 million from Janssen since licensing out Leclaza. In November 2018, Yuhan received a USD 50 million upfront payment for the transfer of Leclaza’s technology. In April 2020, Yuhan received a USD 35 million milestone payment from Janssen. At the time, Johnson & Johnson paid Yuhan the additional milestone payment for initiating a clinical trial for the Rybrevant and Leclaza combination. In November 2020, Johnson & Johnson paid an additional USD 65 million milestone to Yuhan Corp when it started subject recruitment for the trial. Yuhan Corp will also receive an additional USD 60 million in technology fees for the FDA’s approval of Leclaza. Of the total license fee revenue, 40% is paid to the original developer, Oscotec. In 2016, the company acquired the rights to develop the preclinical drug Leclaza from Oscotec and its subsidiary Genosco. The total value of the agreement had been KRW 1.5 billion. Of the amount, KRW 1 billion was set to be paid within 30 days of the signing of the agreement and KRW 500 million was to be paid after the approval of Phase I clinical trials. Additional milestone payments of up to USD 740 million (KRW 984.2 billion) still remain as future development and sales milestones for Leclaza. Yuhan Corp is also currently independently conducting a global Phase III clinical trial for Leclaza. Janssen did not participate in the trial.
- Company
- Will the high-priced Hemgenix be reimbursed in Korea?
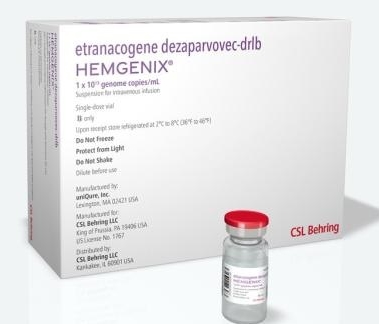
- by Whang, byung-woo Sep 23, 2024 05:50am
- The reimbursement listing process for Hemgenix (etranacogene dezaparvovec-drlb), a 'one-shot' treatment for hemophilia B that shows its effect as a single dose that received domestic approval recently, has been gaining attention in Korea. Pic of Hemgenix According to industry sources on the 21st, the Ministry of Food and Drug Safety (MFDS) recently approved CSL Behring Korea's hemophilia B gene therapy Hemgenix for the treatment of hemophilia B in adults. Hemgenix is used to treat moderate-to-severe hemophilia B (congenital blood clotting factor IX deficiency) in adults without a history of Factor IX inhibitors. Hemophilia is divided into two types, hemophilia A and hemophilia B, based on differences in the distribution of blood clotting factors VIII and IX, and the treatment approach differs depending on the type. Hemophilia B is a congenital bleeding disorder caused by a single gene defect and is caused by a deficiency in coagulation factor IX (blood coagulation factor 9), a protein that helps blood coagulation and is mainly produced in the liver. According to the 2019 White Paper on Hemophilia, the total number of hemophilia patients in Korea was 2,509, of which 1,746 (69.6%) were hemophilia A and 434 hemophilia B patients. Hemgenix delivers a functional gene that activates the production of blood clotting factor IX, enabling patients to produce factor IX on their own, and can reduce bleeding continuously in the long term with just a single injection. The recent availability of extended half-life therapies for hemophilia B has increased the convenience of prophylaxis. While the standard half-life therapies required 104 days of administration per year (based on twice-weekly infusions), the newer extended half-life agents are administered once every 7 to 14 days. However, the newer therapies have limitations despite the increased convenience due to the need for continuous treatment and the unavailability of a cure. In this context, the company is expected to apply for Hemgenix’s reimbursement focusing on the fact that it only needs to be administered once. According to industry sources, CSL Behring Korea is preparing to apply for reimbursement of Hemgenix. The company is expected to apply as early as the first half of next year. In the US, the drug is priced at KRW 4.7 billion (USD 3.5 million), making it virtually impossible for patients to pay on their own, so the company’s reimbursement challenge was naturally the next step. A pharmaceutical industry insider said, “There is a consensus among industry insiders that it would not be easy for CSL Behring Korea to receive reimbursement due to Hemgenix’s very high price. However, as the benefits provided by the drug are clear, the company will likely take a multifaceted approach for its reimbursement in Korea.” If and when the company applies for reimbursement, it is expected to emphasize Hemgenix’s role as a one-shot treatment. While hemophilia B may not be considered life-threatening, patients can die from cerebral or organ bleeding, therefore the company may appeal to the drug’s value as a next-generation treatment that prevents the risks associated with regular intravenous infusions. “Hemgenix offers a unique and innovative approach that enables patients to produce their factor XI, and can fundamentally change the hemophilia treatment paradigm,” said Ki-Woon Kim, CEO of CSL Behring Korea. The issue is in its price. CSL Behring Korea's other hemophilia B drug, Idelvion (albutrepenonacog alfa), is priced at KRW 1,800 per IU/vial, from the lowest 250 IU/vial to the highest 2,000 IU/vial. Hemgenix’s dose is first determined based on age (below 12 or 12 years and older) and then applied a formula to determine the dosage based on body weight. For example, an 80kg patient with severe hemophilia B whose levels are approximately 50% of the normal level would require 3,080 IU of treatment. Simple calculation shows that this translates to 17.4 doses of Idelvion per year, which is a significant difference when comparing the U.S. drug price, even when considering its lifelong use. However, there are variables, such as the fact that the ultra-high priced drugs listed in Korea were given a price lower than those abroad. “At this point, we believe the biggest hurdle in reimbursement will be the burden of drug price on Korea’s national health insurance finances,” said a pharmaceutical industry official. “We expect CSL Behring Korea's track strategy and how convincing the therapeutic benefit and need of Hemgenix is to the government will be the key to its reimbursement in Korea.”