- LOGIN
- MemberShip
- 2026-04-26 15:16:24
- Policy
- First lot of returning nasal spray flu vaccine approved
- by Lee, Tak-Sun Sep 30, 2025 06:12am
- FluMist labelThe nasal spray flu vaccine ‘FluMist Intranasal Spray (AstraZeneca Korea)’ has received shipment approval from the Ministry of Food and Drug Safety (MFDS) and is preparing for sales. This product was previously sold by GC Biopharma, but it did not gain significant popularity at the time. With expected demand from children who dislike injections, attention is on whether it will avoid repeating its past failure. On the 26th, the Ministry of Food and Drug Safety granted shipment approval for FluMist Intranasal Spray (live attenuated influenza vaccine), lot number YK2763C (expiration date January 8, 2026). This is the first shipment approval since it was licensed in April this year, signaling the start of full-scale supply ahead of the flu season. FluMist Intranasal Spray is a trivalent vaccine preventing three viruses (influenza A H1N1, H3N2, and influenza B Victoria). It can be administered to children and adults aged 24 months to 49 years. Safety has not been established for children under 24 months. For those aged 50 and older, administration is prohibited in high-risk groups with underlying conditions, as the incidence of pharyngitis was higher compared to placebo. Nevertheless, this vaccine is gaining attention because it offers convenience in administration, particularly for children who dislike injections. This vaccine is a spray product that delivers the solution into the nose, which is expected to improve acceptability among children and make administration easier for providers. At a press conference celebrating the vaccine’s approval in June, Professor Yoon-Kyung Kim (Pediatrics, Korea University Ansan Hospital) said, “FluMist is a painless vaccine delivered by nasal spray that can contribute to increasing flu inoculation rate among children.” However, as it is not included in the National Immunization Program (NIP), demand is expected to fluctuate depending on pricing. When GC Biopharma launched the product in 2009, demand was low because it cost KRW 5,000–10,000 more than injectable vaccines. As a result, its license was revoked in July 2020 after the validity period expired. Another barrier is that intranasal vaccines are not yet familiar to the public, which could also affect uptake. Still, expectations remain that it could raise pediatric flu vaccination rates and contribute to herd immunity, thereby protecting the elderly from infection. A pharmaceutical industry official said, “Ultimately, pricing will impact sales volume. But unlike in the past, there is now demand for non-reimbursed vaccines that emphasize quality, so if the price gap is small, FluMist could gain a foothold in the market.”
- Company
- Three Korean Pharmas avoid Equfina patent
- by Kim, Jin-Gu Sep 30, 2025 06:12am
- Generic companies have succeeded in avoiding the patent of Eisai Korea’s Parkinson’s disease treatment Equfina (safinamide). With early generic launches drawing closer, competition for the first-generic exclusivity among patent challengers is expected to intensify. According to industry sources on the 29th, the Intellectual Property Trial and Appeal Board recently ruled in favor of three companies—Bukwang Pharm, Myung In Pharm, and Samil Pharmaceutical—by granting their requests for a negative scope confirmation trial against NurrOn Pharmaceuticals concerning Equfina’s patent (No. 10-1491541). Equfina is Eisai Korea’s adjunctive therapy for patients with idiopathic Parkinson’s disease experiencing motor fluctuations. It is used alongside levodopa-containing regimens. The patent holder is NurrOn Pharmaceuticals. Two patents related to Equfina are listed in the Ministry of Food and Drug Safety’s green list. Of these, the “method of treating Parkinson’s disease” patent expired in December last year. The patent expiring in 2028 has now been avoided by generics, and this recent victory reduces the burden for patent challengers applying for generic product approvals. The three companies that successfully avoided the patent are expected to compete for exclusive marketing rights. They have simultaneously satisfied two of the three requirements for obtaining exclusive rights: ‘filing the first patent invalidation petition’ and ‘winning that petition’. If they meet the remaining requirement of ‘being the first to apply for generic approval’, they can monopolize the generic market and exclusively sell their generics for 9 months. Among them, Myung In Pharm is known to be closest to securing exclusivity. The company began a bioequivalence trial in July and has already completed subject enrollment. Bukwang Pharm received approval for a bioequivalence study earlier this month. Samil Pharm has not yet initiated such a trial. All three companies have strong CNS portfolios, suggesting intense competition upon their generics’ launch. Given that the drug is used as adjunctive therapy with levodopa, synergy with existing products is also anticipated. Myung In Pharm already markets Parkinson’s treatments such as Myungdopar (levodopa/benserazide), Perkin (levodopa/carbidopa), and Trilevo (levodopa/carbidopa/entacapone). Samil Pharm sells Onedopa (levodopa/benserazide). Bukwang Pharm launched the schizophrenia/bipolar disorder drug Latuda last year, strengthening its CNS portfolio. Equfina is a third-generation MAO-B (monoamine oxidase-B) inhibitor that acts on both dopaminergic and non-dopaminergic pathways. Eisai received marketing approval in Korea in June 2020 and launched with reimbursement in February 2021. Import sales grew from USD 770,000 in 2021 to USD 2,070,000 in 2023, a 2.7-fold increase in just 2 years.
- Company
- ‘Need to strengthen access to NMOSD treatments’
- by Son, Hyung Min Sep 30, 2025 06:12am
- Rep. Mi-hwa Seo (Democratic Party of Korea, Health and Welfare Committee), Korea NMOSD Patients’ Association, and the Korea Organization for Rare Diseases held a policy discussion forum at the National Assembly on improving access to neuromyelitis optica treatment. On the 25th, Rep. Mi-hwa Seo (Democratic Party of Korea, Health and Welfare Committee) held a policy forum at the National Assembly Hall to strengthen treatment access for neuromyelitis optica spectrum disorder (NMOSD). The forum was co-hosted by Rep. Seo, the Korea NMOSD Patients’ Association, and the Korea Organization for Rare Diseases. NMOSD is a rare disease where even a single relapse can lead to irreversible disabilities like blindness or paralysis. However, domestic reimbursement criteria require conditions such as experiencing two or more relapses within a year after using ‘MabThera (rituximab)’, meaning patients must experience a relapse before they can use the new drug. This has drawn criticism from both patients and experts. This forum was held to address these systemic limitations and discuss ways to expand early treatment access. In the first presentation, Professor Ki-hoon Kim of the Department of Neurology at Severance Hospital, pointed out the issues present in the domestic reimbursement environment through the ‘Proposals for Improving Treatment Accessibility for Neuromyelitis Optica Spectrum Disorder.” Professor Kim said, “Although these therapies can prevent relapses, the unreasonable reimbursement criteria prevent patients from accessing them early. Early use of new drugs must be guaranteed to prevent unnecessary relapses and the accumulation of disabilities.” Patient Bo-ram Park followed with a presentation conveying patients' realities through ‘A Relapse-Free Life and Challenges for Early Treatment: Insights from Patient Experience’. Park appealed, “After a long diagnostic odyssey, treatment begins, but patients often resort to off-label drugs or discontinue treatment due to side effects. While there are new drugs with a 0% relapse rate, they remain outside the reimbursement scope, leaving patients at continued risk of relapse.” The subsequent panel discussion was chaired by Professor Yong-jin Kwon of Seoul National University Hospital's Public Healthcare Center. Participants included: ▲ Jong-cheol Choi, caregiver for a patient with neuromyelitis optica spectrum disorder (NMOSD); ▲Eung-gyu Park, caregiver for a patient with NMOSD; ▲ Yeon-sook Kim, Director of the Pharmaceutical Benefit Division at the Ministry of Health and Welfare; ▲ Kook-Hee Kim, Director-General of Pharmaceutical Management at the Health Insurance Review and Assessment Service (HIRA); and ▲Yoon-Ho Eo, Dailypharm reporter, who discussed directions for improving the system for NMOSD. Participants highlighted common goals: alleviating patient and caregiver suffering caused by repeated relapses, introducing relapse-preventing drugs at earlier stages, and improving reimbursement standards to reduce long-term care and treatment costs. Rep. Seo concluded, “Although NMOSD has only been recognized as an independent disease for about 20 years, advances in medical technology now allow us to prevent relapse-related disabilities. Major countries have already reformed their systems so patients can use approved therapies from the outset. Korea must also make institutional improvements so patients don’t have to endure unnecessary relapses.”
- Policy
- MFDS, GLP-1 obesity drug + diabetes med combo hypoglycemia↑
- by Lee, Tak-Sun Sep 30, 2025 06:11am
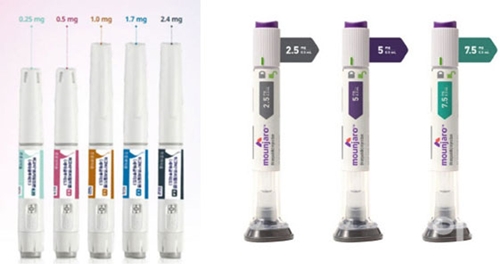
- GLP-1 obesity drugs Wegovy(left) and Mounjaro.The Ministry of Food and Drug Safety (MFDS) announced that patients with diabetes using GLP-1 obesity treatments, which have recently become popular, must consult with their healthcare provider, as the co-administration of these drugs with diabetes medication significantly increases the risk of hypoglycemia. The MFDS also stressed that the use of obesity treatments must be avoided during pregnancy and lactation. Popular GLP-1 obesity drug brands include 'Wegovy' and 'Mounjaro.' The MFDS (Minister Yu-Kyoung Oh) and the Korea Institute of Drug Safety and Risk Management (KIDS)(President Soojung Sohn) announced on September 29 that they have distributed a 'Guidelines to Safe Use of GLP-1 Obesity Treatments' to regional medical associations and drug safety centers nationwide. This guide contains information on ▲the diseases for which the obesity treatments are used ▲correct administration methods, storage and disposal ▲precautions for use ▲reporting of adverse reactions (side effects). GLP-1 obesity treatments are prescription drugs prescribed to: obese patients with an initial Body Mass Index (BMI) of 30kg/m2 or higher, or overweight patients with a BMI of 27kg/m2 to less than 30kg/m2 who have one or more weight-related comorbidities. The MFDS emphasized that patients taking diabetes medication who are also taking GLP-1 obesity treatments are at a higher risk of hypoglycemia and should consult with their healthcare provider about whether to adjust drug dosages. They also added that the use of obesity treatments is prohibited during pregnancy and lactation, and it is advisable to plan pregnancy considering the drug's residual period in the body. Depending on the specific obesity treatment, contraception may be necessary for at least 1-2 months after discontinuing the medication. Obesity treatments should not be started at a high dose immediately. Instead, patients should initiate treatment with the dose specified by their physician, according to the approved regimen, and gradually increase it, strictly adhering to the dosage and administration instructions provided by both the physician and pharmacist. When administering the obesity treatment, patients should inject into the abdomen, thigh, or upper arm, whichever site is most convenient, and rotate the injection site with each dose. Patients must inform their healthcare professional before administration about ▲any known drug hypersensitivity ▲all currently administered medications, medical history ▲whether they are pregnant or breastfeeding. Additionally, obesity treatments should be stored in the refrigerator away from light. If the medication is frozen, contains particles, or has changed color, it should not be used and must be disposed of. The MFDS stressed that even when GLP-1 obesity treatments are used within the approved scope, adverse events such as gastrointestinal disorders, injection site reactions, fatigue, and dizziness can commonly occur. More clinically significant adverse events, such as hypersensitivity reactions, acute pancreatitis, cholelithiasis, and cholecystitis, may also occur. In such cases, patients should notify their healthcare team or visit the hospital. The MFDS stated that GLP-1 obesity treatments, as prescription drugs, must be used strictly following a physician's prescription and a pharmacist's dispensing and guidance, ensuring safe use within the authorized indications for obesity treatment. It was also stressed that purchasing or distributing these drugs through overseas direct purchases or person-to-person sales online should be avoided, as the product's safety cannot be guaranteed. An MFDS official said, "We hope this guide helps patients using GLP-1 obesity treatments to administer their medication safely." The educational material is available on the MFDS website (www.mfds.go.kr) → Law/Data → Promotional Materials → General Promotional Materials section, on the KIDS website (www.drugsafe.or.kr) → Education/Promotion → Resources section.
- Company
- Global stage features changes in drugs for metabolic disease
- by Son, Hyung Min Sep 29, 2025 06:08am
- The International Congress of Diabetes and Metabolism (ICDM 2025) took place from September 25 to 27, 2025, at the Grand Walkerhill Hotel in Seoul, Korea. A promotional competition between Korean and international pharmaceutical companies, highlighting the latest treatments for diabetes and metabolic disorders, unraveled at a recent medical conference in Korea. The International Congress of Diabetes and Metabolism (ICDM 2025), held at the Grand Walkerhill Hotel in Seoul over three days starting September 25, featured a promotion focused on a range of topics, including the latest diabetes treatments, centered on GLP-1 and SGLT-2 inhibitors, as well as kidney disease therapies and vaccines. Bayer, Novo Nordisk, GSK, Boehringer Ingelheim, and Daewoong Pharmaceutical participated as diamond sponsors, taking on the key sponsor roles. GLP-1 Rivals Enter Side-by-Side…Shingles and RSV Vaccines Also Garnered Attention Eli Lilly Korea and Novo Nordisk, two leading companies in the GLP-1 market, participated side by side at the event to promote their respective GLP-1 portfolios. Following products like 'Trulicity (dulaglutide)' and 'Victoza (liraglutide),' both companies are seeking market entry for their newer GLP-1 formulations. (from left) Novo Nordisk and Eli Lilly exhibition booths. Currently, Novo Nordisk has secured domestic approval for 'Ozempic (semaglutide),' and Lilly has secured domestic approval for 'Mounjaro (tirzepatide)' in Korea. These companies have recently completed their applications for insurance reimbursement. Ozempic and Mounjaro are Glucagon-like Peptide-1 (GLP-1) class drugs used in patients with Type 2 diabetes and obesity. These two drugs have demonstrated significant effects in lowering blood sugar and reducing body weight in clinical trials. While the weight loss effect of existing DPP-4 inhibitors or SGLT-2 inhibitors was limited to less than 5%, clinical results showed that GLP-1 formulations can achieve weight loss of 10% or more. Consequently, GLP-1 formulations are increasingly included in the latest global R&D trends. Studies have shown that if diabetic patients lose more than 5% of their body weight, not only are their blood sugar, blood pressure, and lipid levels improved, but the incidence and mortality rates of cardiovascular and cerebrovascular diseases can also be lowered. Both companies also expressed their intent to collaborate with domestic pharmaceutical companies. Novo Nordisk recently initiated a co-promotion for the obesity treatment 'Wegovy (semaglutide)' with Chong Kun Dang, and the possibility of an additional contract for Ozempic is also being discussed. Lilly is currently seeking a co-promotion partner for Mounjaro, and a strategy is anticipated that will utilize a single product name to cover both diabetes and obesity indications simultaneously. In addition to diabetes, companies promoted the management of complications and vaccines at the conference. (from left) GSK and Bayer exhibition booth. Bayer prominently featured its kidney disease treatment, 'Kerendia (finerenone).' Kerendia is a drug that targets mineralocorticoid receptor (MR) overactivation, contributing to the treatment of key chronic kidney disease pathologies and heart failure patients with a left ventricular ejection fraction (LVEF) of 40% or more. Kerendia is currently approved in over 95 countries globally and has recently obtained approval for heart failure patients in the U.S. A subgroup analysis of the CONFIDENCE study, presented at the European Society of Cardiology (ESC) this year, reported high hemodynamic compliance when Kerendia was combined with SGLT-2 inhibitors. GSK focused on promoting its shingles vaccine, Shingrix, and the respiratory syncytial virus (RSV) vaccine, Arexvy. The importance of vaccination was highlighted, considering the frequent opportunities for vaccination in endocrinology clinical settings. Shingrix is a recombinant zoster vaccine that has been shown to have a stronger preventive effect than the existing live attenuated vaccine. Arexvy, which officially launched in Korea this year, attracted attention as the world's first RSV vaccine targeting older adults aged 60 and over. The Market Gap Left by Forxiga...Generics Compete with Jardiance and Envlo The promotional competition among SGLT-2 inhibitors was also heated. Following AstraZeneca's announcement of its withdrawal of the market-leading SGLT-2 inhibitor 'Forxiga (dapagliflozin)' from the Korean market in December 2023, there was intense anticipation that the original drugs 'Jardiance (empagliflozin)' from Boehringer Ingelheim and 'Envlo (enavogliflozin)' from Daewoong Pharmaceutical would gain a significant rebound effect. (upper left, clockwise) Boehringer Ingelheim, Daewoong, HK inno.N, Boryung exhibition booths. Jardiance is highly anticipated for sales growth, as it has secured both the chronic heart failure and chronic kidney disease indications, similar to Forxiga. Consequently, Boehringer Ingelheim focused on promoting Jardiance at this conference. Korean companies prominently featured their generics. HK inno.N, Boryung, and Hanmi Pharmaceutical joined the competition by promoting their Forxiga generics. Among these companies, HK inno.N and Boryung have formed a rivalry for the number one and two spots in market share. After AstraZeneca transferred its indications to HK inno.N's Dapa.N following the withdrawal of Forxiga. Dapa.N rose to become the leader in the monotherapy market. Indeed, Dapa.N recorded KRW 2.3 billion in prescription sales in the first quarter of this year, securing the top spot over Boryung's 'Trudapa' (KRW 1.3 billion), and further widening the gap in the second quarter. Hanmi Pharmaceutical's 'Dapalon' recorded the fourth-largest sales, following HK inno.N, Boryung, and Daewoong Bio, demonstrating its market presence. The competition between the original drugs and generics to fill the void left by Forxiga is now intensifying.
- Opinion
- [Desk’s View] MFDS should clarify AAP safety message
- by Lee, Tak-Sun Sep 29, 2025 06:08am
- Unforeseen moves by U.S. President Donald Trump are having a considerable impact in Korea. After sudden tariff hikes rattled the Korean economy, an unexpected drug safety issue has now emerged. The domestic healthcare market, which is reliant on overseas drugs, is reeling from Trump-related risks. The controversy began on the 22nd when President Trump stated at a press conference that acetaminophen is not safe for pregnant women. He said, “Acetaminophen, widely known as Tylenol, may increase the risk of autism in children if taken during pregnancy. The U.S. Food and Drug Administration will notify doctors of this, and if necessary, recommend restricting Tylenol use during pregnancy.” Acetaminophen, widely known under the brand name Tylenol (Kenvue), is one of the most commonly used fever reducers and pain relievers in Korea. It is generally regarded as relatively safe for pregnant women and young children, which is why healthcare professionals frequently recommend it to such patients. Trump's remarks appear to be based on a recently published report by a research team at the Icahn School of Medicine at Mount Sinai in the United States. This report suggests a possible link between Tylenol use and autism. However, academic communities in Korea and abroad are pointing out that Trump's statement is premature, as scientific evidence linking acetaminophen to autism remains insufficient. The Korean Pharmaceutical Association stated, “Major global health authorities and academic organizations have made it clear that there is insufficient scientific evidence to support such claims at this time.” The Korean Medical Association also dismissed the claims, citing insufficient evidence. KMA spokesman Sung-keun Kim said in a regular briefing, “There is no scientifically established evidence to support the claim that taking Tylenol during pregnancy causes autism in the fetus.” The same sentiment is echoed overseas. WHO spokesman Tarik Jasarevic told reporters at a press briefing, “Evidence remains inconsistent.” The European Medicines Agency (EMA) also stated in a release, “Based on the evidence available to date, no association has been found between the use of paracetamol (the active ingredient name for acetaminophen in Europe) during pregnancy and autism.” However, confusion persists as the US Food and Drug Administration (FDA), the regulatory authority for Tylenol’s home country, has yet to issue an official statement. The stance of the Ministry of Food and Drug Safety (MFDS) is also ambiguous. While the MFDS stated it would receive relevant data from manufacturers and discuss the matter, it has not issued a clear message. It did note, however, that under current approval guidelines, if a pregnant woman experiences a persistent fever above 38°C in early pregnancy, it could affect fetal neural development. In such cases, acetaminophen-based fever reducers and pain relievers may be taken, but the dosage should not exceed 4,000 mg per day. It added that since individual medical situations may vary, pregnant women should consult a healthcare professional before taking any medication containing acetaminophen. This reflects a cautious stance regarding the link between acetaminophen use during pregnancy and autism. This is understood to be a comprehensive reflection of the lack of official statements from the U.S. President, a key ally, and the FDA. Nevertheless, compared to the WHO and EMA stating there is still no clear evidence, this stance appears overly passive. Furthermore, the title of the official press release, “Consult a healthcare professional and take as directed,” seems to shift the burden onto private experts rather than the government. Had the government clearly communicated that, at least for now, evidence is insufficient and that the drug should be taken according to current approved guidelines, it would have alleviated public anxiety. The Ministry of Food and Drug Safety (MFDS), despite being a regulatory body like the FDA or EMA, has faced significant criticism in the past for making decisions based on politics rather than scientific evidence. Of course, it is not entirely independent from government influence, and unlike the FDA or EMA, it lacks manpower and expertise; therefore, direct comparisons may not be fair. Nevertheless, if Korea is to be recognized as a member of the advanced nations and if MFDS truly seeks global recognition as a competent regulatory agency—as it often promotes—then in such controversies, it must deliver clearer, science-first messages. That would undoubtedly strengthen public trust in MFDS by showing that science is prioritized over politics.
- Policy
- MoHW and NHIS agree on need to expand expedited listing
- by Jung, Heung-Jun Sep 29, 2025 06:08am
- The Ministry of Health and Welfare (MoHW) expressed consensus on the need to expand fast-track reimbursement to improve access to treatments for rare and severe diseases. As the government agenda already includes system improvements to reflect the innovative value of new drugs, the ministry stated its intent to support these reforms. On the 26th, at a forum on improving the operation of the National Health Insurance finance hosted by Representatives Mi-hwa Seo and Jong-tae Jang, the government, industry, and academia all voiced the need to expand fast-track reimbursement for rare disease treatments. Yeon-sook Kim, Director-General of the Pharmaceutical Management Division at MOHWYeon-sook Kim, Director-General of the Pharmaceutical Management Division at MOHW, said, “Rare and severe diseases are difficult to diagnose, and the small patient population leads to insufficient data. We do regret how the listing process takes a long time, and communication regarding system improvements has been slow. We will gather opinions to develop the system rationally.” Kim added, “This is also included in the government's national agenda. We have decided that the drug pricing system will support the creation of an ecosystem for innovative new drug development by reflecting the innovative value of new drugs. This also includes alleviating the burden of rare and intractable diseases.” "Our goal is to ensure that more necessary drugs are covered quickly through expedited listing and to broaden coverage. Currently, we are also attempting to accelerate the process by concurrently handling approval and listing. The national agenda also comprehensively includes improvements to the drug pricing system. However, as it requires significant social consensus and careful consideration, we will need time to discuss improvement measures." The National Health Insurance Service (NHIS) emphasized the need for a roadmap to prioritize reimbursement and use resources more efficiently. Yoo-kyung Yoon, Director of Pharmaceutical Management at NHISYoo-kyung Yoon, Director of Pharmaceutical Management at NHIS, said, “There are limitations in terms of budget and review manpower, but I agree expansion is necessary. We recognize the importance of prioritization. We need to review reimbursed drugs, set reimbursement priorities, and establish a roadmap for efficient fiscal use.” “We must determine how to select drugs eligible for fast-track, identify issues as the system is implemented, and continuously improve it to ensure prompt reimbursement can be achieved. Adjusting the reimbursement scope requires social consensus, so we will thoroughly gather opinions from stakeholders.” Yoon also emphasized, “Improvements to the generic drug pricing system must also be considered alongside measures to foster a virtuous cycle in the industry. Rapid listing of rare and intractable disease drugs is included in national policy tasks, and we will strive to develop solutions.” The industry expressed that establishing a virtuous cycle structure is urgently needed to enable the development of innovative new drugs for rare and severe diseases. Jae-won Heo, Executive Director at Gilead Sciences Korea Jae-won Heo, Executive Director at Gilead Sciences Korea, noted, “Hepatitis C, which can progress to liver cancer, already has curative treatments. If patients are treated early, it can actually reduce the financial burden on the NHIS. Data also shows that 20% of cancer patients give up economic activity, devoting much of their time to caregiving. Supporting their return to society carries significant value.” Heo explained, “The number of patients is small, but development is extremely difficult, and companies inevitably face heavy burdens. Even after more than 10 years of research, it is not uncommon to see results showing no clinical effect. Despite failures, companies continue to develop treatments because patients exist. A virtuous cycle must be established so development is feasible,” urging expansion of new drug access. Professor Yong-jin Kwon of Seoul National University Hospital Criticism also emerged that the government should not show a passive attitude toward coverage for rare and severe diseases, and that Aative review of the generic drug pricing system is also necessary. Professor Yong-jin Kwon of Seoul National University Hospital's Public Healthcare Center pointed out, "New drugs are approved, but they aren't even used as non-reimbursed treatments, so they don't show up in the statistics. The coverage rate appears high, but that's because no treatment exists. In reality, the coverage rate for rare diseases isn't high. Furthermore, care costs are not factored in.“ Kwon further criticized, “NHIS does not examine how much value has been generated (so far) from the high prices paid for generics and the development of innovative R&D treatments. How much have domestic pharmaceutical companies advanced over the past 25 years? We need to evaluate the outcomes and discuss the development of the pharmaceutical industry.” stressing the need to reform the generic pricing system.
- Policy
- “Cut prices of generic drugs across the board”
- by Jung, Heung-Jun Sep 29, 2025 06:07am
- A proposal has been made to establish reimbursement priority for treatments targeting rare/serious diseases versus mild conditions, thereby expanding access to new drugs. There were also calls to reform the distorted pharmaceutical budget structure by cutting generic prices across the board and canceling approvals for products lacking bioequivalence data. At a National Assembly forum on improving the operation of health insurance finances for rare and severe diseases, hosted on the 26th by lawmakers Mi-hwa Seo and Jong-tae Jang, participants stressed the need to allocate limited insurance resources more effectively to improve access to new drugs. Prof. Yong-jin Kwon of Seoul National University Hospital’s Public Healthcare Center Professor Yong-jin Kwon of Seoul National University Hospital’s Public Healthcare Center said, “The National Health Insurance system has reached a structural contradiction. While pharmaceutical spending exceeds the OECD average, access to innovative drugs remains restricted, depriving patients of treatment opportunities. Coverage for rare and severe diseases should have expanded, but instead, it has regressed.” Professor Kwon called for ▲Reestablishing reimbursement priorities, ▲reforming the drug management system , and ▲expanding access to new drugs. He explained that a survey conducted last July of 1,000 citizens showed significant public agreement on prioritizing coverage for patients with rare and severe diseases. According to the results, 46.7% agreed with prioritizing severe disease patients, and 52.7% supported prioritizing rare disease patients. However, 76.9% responded that while premiums should be maintained at the current level, coverage should be differentiated. Prof. Kwon said, “This suggests there is sufficient basis to regard reprioritization as being highly feasible.” Professor Kwon proposed the following improvement measures ▲establishing a National Health Insurance Priority Committee with public participation ▲implementing blanket price reductions for generic drugs and fostering competition, and ▲introducing a fast-track system for rapid listing and flexible benefit determination. Prof. Kwon said, “The share of pharmaceutical expenditures is already high, but the portion spent on new drugs is low. The generic market is driving distortion. We should consider whether this is due to high prescription volumes or high generic prices,” stressing the need to shift reimbursement priorities from mild to severe conditions. He added, “Prioritization should consider disease severity and social costs, as well as risks of treatment delays and potential market failures.” He also argued that generic drug prices should be cut across the board, and generics lacking bioequivalence testing should have their approvals revoked. He stated, “It is unworthy of our national standing that drugs without bioequivalence certification are still circulating. Bioequivalence test results should be made public. Citizens must be convinced that the efficacy and composition are identical.” Furthermore, he called for expanding fast-track reimbursement and flexible decision-making for rare disease drugs. Suggestions included accelerating reviews, granting conditional approvals, and enhancing post-marketing management through fast-track pathways. He concluded, “We must streamline the health technology assessment process and implement conditional approvals. If MFDS approval represents the product, insurance reimbursement represents the technology. Even if not yet officially authorized, reimbursement should be possible based on technological appropriateness. For rare diseases, conditional approval and reimbursement must be adopted, and real-world evidence (RWE) should be leveraged for more sophisticated post-market management.” He added, “Flexible reimbursement frameworks must be expanded. Risk-sharing agreements (RSA) should be applied diversely, such as on a performance-based basis. Patients should also understand that the limited coverage can be gradually expanded over time.”
- Company
- CKD and Kwang Dong win Tagrisso formulation patent suit
- by Kim, Jin-Gu Sep 26, 2025 06:14am
- Generic drugmakers challenging AstraZeneca's patent for the non-small cell lung cancer treatment ‘Tagrisso (osimertinib)’ have won their case in the first instance. According to industry sources on the 25th, the Intellectual Property Trial and Appeal Board (IPTAB) on the 24th ruled in favor of Chong Kun Dang and Kwang Donng Pharmaceutical in their request for a negative right scope confirmation trial regarding Tagrisso’s formulation patent (No. 10-2336378). This significantly increases the possibility of an early launch of Tagrisso generics. The two companies have also met 2 key requirements for obtaining exclusive marketing rights (first generic exclusivity): ▲ being the first to file the trial request and ▲ winning the trial/litigation. Now, they only need to satisfy the condition of being the first to file for generic approval to obtain the first generic exclusivity right. CKD and Kwang Dong are the only companies to have challenged the Tagrisso formulation patent. If both secure the first approval for their generics and gain the first generic exclusivity rights, they will be able to sell their product exclusively for 9 months. The key variable is AstraZeneca’s appeal. If AstraZeneca files a lawsuit to overturn the IPTAB decision with the Patent Court, the dispute may be prolonged. AstraZeneca's decision on whether to appeal has not yet been made. Tagrisso is protected by three patents: substance patents expiring in November and December 2033, and a formulation patent expiring in January 2035. CKD and Kwang Dong have successfully avoided the formulation patent. With the formulation patent out of the way, both companies plan to launch their generics as soon as the substance patent expires in 2033. There is also speculation that they could aim for an even earlier launch by targeting the extended duration granted to the substance patent. Tagrisso is a targeted anticancer drug used for EGFR-mutated non-small cell lung cancer (NSCLC) that received domestic approval in 2016. It is used as a first-line treatment for patients with locally advanced or metastatic NSCLC harboring EGFR gene mutations. In Korea, it competes with Yuhan Corp’s Leclaza (Lazertinib). According to the market research institution IQVIA, Tagrisso’s sales in Korea reached KRW 111 billion in 2023. After surpassing KRW 100 billion in annual sales in 2022, growth has continued steadily. With reimbursement expanded last year to include first-line treatment for locally advanced and metastatic NSCLC patients with specific EGFR mutations, sales are estimated to have exceeded KRW 130 billion. Separately, CKD is developing its own new drug for non-small cell lung cancer. The candidate compound, named ‘CKD-702’, is a bispecific antibody targeting both cMET and EGFR. It is currently undergoing global Phase I clinical trial. CKD is seeking to strengthen its foothold in the NSCLC treatment market by developing both a new drug and a generic.
- Opinion
- [Reporter’s View] The gap between innovation and access
- by Son, Hyung Min Sep 26, 2025 06:12am
- Advances in medicine have created pivotal turning points in the course of human survival. Diseases once deemed incurable are gradually being reclassified as chronic conditions. From anticancer drugs to treatments for rare diseases and immunotherapies, innovative new drugs have not only prolonged patients’ lives but also increased the burden of responsibility borne by nations and societies. The problem lies in the fact that the ‘pace of innovation’ and the ‘pace of patient access’ are not on the same track. Korean patients are always left to wait. Even when news arrives that a new drug has been approved in the US or Europe, a gap of 1 to 3 years often exists before patients can actually receive a prescription domestically. This delay is not merely a procedural issue; it represents a lost opportunity for treatment. For a terminal cancer patient, 1 year can be their entire life. This is why it's not uncommon for patients to seek treatment abroad. At the center of this irony lies a uniquely Korean formula: price over innovation. The value of a new drug is first calculated by its burden on the national health insurance budget rather than by its clinical significance and impact on patient survival. While managing insurance finances is clearly a crucial task in national governance, the balance has tilted excessively toward fiscal restraint, depriving patients of the opportunity to timely benefit from innovations. This is also why pharmaceutical companies often push Korea down the priority list in their global launch strategies. The so-called ‘Korea passing’ concern is not an abstract warning but a real risk that delays actual patients' treatment opportunities. The global environment is not favorable either. President Trump’s MFN (Most Favored Nation) drug pricing policy has posed a threat to pricing systems worldwide. Under the pretense of protecting American patients, it targeted countries like Korea that maintain low drug price systems as risk factors. From the perspective of multinational pharmaceutical companies, the incentive to launch drugs in Korea has diminished because protecting prices in the US market has become more critical. In other words, Korea’s low drug prices translate directly into being deprioritized in global market strategies. This leads us to a fundamental question: what is a new drug to the patient? To the government, it may be a budget variable; to companies, a profit variable. But to patients, a new drug is a survival variable. Unless the perspective shifts from “how cheaply can we bring it in” to “how quickly and fairly can it reach patients,” the meaning of innovation becomes powerless in front of patients. Of course, the constraints of the national health insurance budget are an undeniable reality. Within limited resources, it's difficult to unconditionally recognize the value of new drugs and raise their prices. The government isn't sitting idle either. New attempts are being discussed, such as the approval-evaluation linkage pilot project, expansion of risk-sharing schemes, and recently, indication-based pricing. But the fundamental limitations remain. Within the current system, patient access to new drugs inevitably remains low. A radical policy shift is now needed. So what constitutes as ‘radical’? Suggestions include introducing value-based assessment that prioritizes clinical innovation and patient survival outcomes; implementing multi-layered risk-sharing schemes where government, pharmaceutical companies, and society share burdens; and establishing a national strategy vision that enhances international negotiation power and improves patient access. Furthermore, a paradigm shift is needed—one that recognizes healthcare not merely as a fiscal issue, but as a core national competitiveness factor. Medical innovation will not cease. The problem is that the speed at which this innovation reaches Korean patients remains sluggish. How long can we tolerate the paradox of patients lagging behind in this era of innovation? Now is the time for government, industry, and society to find answers together. A decisive policy action to align the speed of innovation with patients’ needs is urgently required—so that patients no longer have to waste their time waiting.