- LOGIN
- MemberShip
- 2026-04-28 15:52:43
- Company
- Jeil’s super-antibiotic cefiderocol approved in Korea
- by Nho, Byung Chul Feb 20, 2025 05:59am
- Jeil Pharmaceutical (CEO Seok-je Sung) announced on the 19th that it has received approval from the Ministry of Food and Drug Safety to market the drug Fetroja Inj 1g’ (cefiderocol sulfate tosylate) for the treatment of multidrug-resistant gram-negative bacterial infections. With the approval, adult patients may use Fetroja for the treatment of the following infections caused by susceptible Gram-negative microorganisms: • Complicated Urinary Tract Infections (cUTI), including Pyelonephritis • Hospital-acquired Bacterial Pneumonia and Ventilator-associated Bacterial Pneumonia (HABP/VABP) Prior to this domestic approval, Fetroja Inj has been approved in more than 10 countries around the world, including the US, Europe, and Japan, and was designated by the Ministry of Food and Drug Safety as a national essential medicine in April 2024 as a medicine necessary for responding to public health crises and promoting public health. Fetroja Inj, which was developed by Shionogi, is the world's first siderophore cephalosporin antibiotic, it binds with iron and is then absorbed into the cell through the bacteria's iron-porin channels to overcome the problem of existing antibiotics losing their effectiveness due to resistance. Through this different mechanism of action, it shows a strong antibacterial effect, and Jeil Pharmaceutical expects it to present new possibilities in the treatment of infections caused by multidrug-resistant pathogens that have been difficult to effectively treat with existing treatment options. Fetroja Inj demonstrated in-vitro activity against various antibiotic-resistant (AMR) pathogens, including carbapenem-resistant enterobacteriaceae (CRE), carbapenem-resistant acinetobacter baumannii (CRAB), and carbapenem-resistant pseudomonas aeruginosa (CRPA) that produce metallo-beta-lactamase (MBL). A Jeil Pharmaceutical official said, “Fetroja is an innovative antibiotic that was named to conquer pathogens by using the Trojan horse mechanism of penetrating pathogens through the iron (Fe) forin channel. It will be an important treatment option for patients with complicated urinary tract infections, including nephropyelitis, and ventilator-associated pneumonia, which was difficult to treat due to multidrug-resistant bacteria infection.” Jeil Pharmaceutical signed an exclusive domestic supply agreement with Ping An-Shionogi in July 2022 and secured the rights to develop and commercialize ‘Fetroja Inj.’ Meanwhile, Shionogi is a global research-oriented pharmaceutical company established in 1878, and has a long history and expertise in the development of infectious disease treatments. In particular, it is conducting continuous research and development in the fields of antibiotics, antiviral drugs, and central nervous system treatments, and currently has subsidiaries in Japan, the United States, Europe, and China. Ping An-Shionogi was established in 2020 as a joint venture between the Japanese company Shionogi and the Chinese company Ping An, and introduced the Asian rights to “Fetroja Inj.” However, in December 2024, Shionogi acquired all of Ping An's shares and incorporated it as a subsidiary of Shionogi.
- Company
- Myelofibrosis drug 'Omjjara' attempts at reimb listing
- by Eo, Yun-Ho Feb 20, 2025 05:59am
- 'Omjjara,' a targeted treatment for myelofibrosis, attempts to be added to the National Health Insurance reimbursement list. According to industry sources, GSK Korea submitted a reimbursement application for its new myelofibrosis drug, Omjjara (momelotinib), at the end of last year, and is awaiting to be considered for the Health Insurance Review and Assessment Service (HIRA)'s Cancer Disease Review Committee (CDRC). The company has applied for the indication to treat 'adult patients with intermediate or high-risk myelofibrosis who have anemia.' The drug has approved indications to treat primary myelofibrosis, post-polycythemia vera myelofibrosis, or post-essential thrombocythemia myelofibrosis. Unlike single-target drugs, Omjjara is a multi-target drug that blocks three key signaling pathways. It is expected to have a significant treatment effect. This drug has an inhibitory ability along three key signaling pathways, including JAK1 and JAK2 proteins that are targets of previous drugs, along with activin A receptor type 1 (ACVR1). The recommended dosage is once daily oral administration of 200 mg, and it can be taken regardless of meal intake. Myelofibrosis is a rare blood cancer in which the buildup of fibrosis in the bone marrow causes symptoms such as anemia, thrombocytopenia, and enlarged spleen and liver. It occurs in 1 out of 100,000 worldwide. In South Korea, it has been reported that as of 2023, about 2292 patients have received inpatient and outpatient treatments. Patients who have anemic symptoms have poor prognosis after treatment, and the problem is most patients experience anemia. According to the research, 87% of myelofibrosis patients were reported to be anemic at the time of diagnosis. In another study, 46% of patients required blood transfusion after one year of diagnosis. Typically, anemia in myelofibrosis patients increases the death risk by twofold compared to other prognostic factors, such as age, increased white blood cells, and symptoms throughout the body. The clinical efficacy and safety profile of Omjjara were confirmed through the Phase 3 'SIMPLIFY-1 study' and 'MOMENTUM study.' The studies confirmed that the drug improved key symptoms, such as enlarged spleen, in adult myelofibrosis patients and reduced dependence on blood transfusions in anemic patients. Firstly, the SIMPLIFY-1 study directly compared Omjjara to 'Jakavi (ruxolitinib)' in 432 adult myelofibrosis patients without prior JAK inhibitor therapy. Subgroup analysis was performed in patients with anemia. The results showed that Omjjara was confirmed to be non-inferior to ruxolitinib in terms of the primary efficacy endpoint, which was a spleen volume at week 24 (≥35% reduction). Non-inferiority was not identified in the total symptom improvement score. The rate of transfusion independence in each patient group was confirmed. The rate of patients with transfusion independence in the Omjjara treatment group was 66.5%, and those in the ruxolitinib treatment group were 49.3%, showing that the Omjjara treatment group had significantly lower transfusion independence. In the MOMENTUM study, which was another basis of approval, the efficacy and safety of Omjjara to 'danazol' were compared in 195 adult patients with myelofibrosis who had previously undergone JAK inhibitor therapy, exhibited symptoms, and had anemia. All study participants had been treated with ruxolitinib before, and 4.6% of the patients received 'fedratinib.' The common primary efficacy endpoint was the percentage of patients with a 50% or greater reduction in the Total Symptom Score (TSS) and transfusion independence at week 24.
- Company
- Organon Korea releases first product after spinoff
- by Whang, byung-woo Feb 20, 2025 05:58am
- Organon Korea is launching a new product for the first time since its spin-off in June 2019 and is beginning to expand its influence in earnest. The product, which was unveiled about 3 years after the official launch of the Korean subsidiary, is JADA, a medical device used to control and treat postpartum hemorrhage. The company plans to target the market with its women-focused strategy that differentiates itself from other companies. At a media session held on the 19th, the company announced the launch of JADA and expressed Organon's commitment to improving women's health and safe birthing environments in this era of low fertility. JADA is a new technology that has emerged 15 years after the previously used “intrauterine balloon tamponade and compression suture.” In the case of intrauterine balloon tamponade and compression, hemostasis was achieved by directly applying pressure to the inner wall of the uterus for 12 to 24 hours, but JADA induces physiologic contraction by creating a negative pressure in the uterus within a few minutes and applying pressure (up to 90 mmHg). In the PEARLE trial, 94% of patients could control postpartum hemorrhage without additional treatment, and the median time taken to control their bleeding was 3 minutes. In March of last year, JADA was approved by the Ministry of Food and Drug Safety to control and treat abnormal postpartum hemorrhage when conservative management of the uterus is required. In June of the same year, intrauterine negative pressure hemostasis using JADA was listed as a new health technology based on the results of the safety and effectiveness evaluation of new health technologies by the National Evidence-based Healthcare Collaborating Agency (NECA). Jada's indication, postpartum hemorrhage, is a condition with a high unmet need in women's health worldwide, and it is one of the complications of childbirth that occurs in one in six mothers worldwide, highlighting the need for immediate and appropriate treatment. On this day, Professor Geum Joon Cho of the Department of Obstetrics and Gynecology at Korea University Guro Hospital explained, “One of the main causes of postpartum hemorrhage is uterine atony. A normal uterus naturally stops bleeding through contraction after childbirth, but in the case of uterine atony, the contraction does not occur properly, so the bleeding continues. If the bleeding is not controlled with initial treatment, an intrauterine device is inserted to try to stop the bleeding.” Professor Cho added, “In Korea, as of 2021, labor and delivery complications account for 34.8% of the causes of maternal mortality, and any postpartum hemorrhage that may occur in connection with this should be treated immediately.” He also emphasized, “For mothers experiencing postpartum hemorrhage, prompt judgment by on-site medical staff and the use of appropriate medical devices are very important.” Professor Cho explained that JADA is meaningful in that it provides a new treatment option that can quickly and accurately control postpartum hemorrhage, in the current situation where there is a high level of interest in maternal health due to the low birth rate issue. Professor Cho said, “NECA has been evaluated as having an acceptable safety profile, a high treatment success rate, and an effectively low volume of transfused blood, so it is worth trying by clinicians.” Meanwhile, this launch is significant in that it marks the beginning of the company’s movement to specialize in solutions that are specifically designed for women's health, which has been a key focus of Organon Korea since its inception. Jung Eun Jang, Country Medical Director at Organon Korea, said, “Since Organon was launched with the vision of promoting women's health, we have been continuously striving to provide a wider range of choices by providing various solutions to treat diseases that occur only in women or are disproportionately affected and have unique effects on women.” So Eun Kim, Managing Director of Organon Korea, added, “Postpartum hemorrhage is a problem that can affect not only the mother but also the unborn child, the family, and society as a whole. We hope that the launch of this product will create an environment where postpartum hemorrhage can be treated more quickly and effectively.”
- Company
- Celltrion’s Prolia and Xgeva biosimilars approved in Europe
- by Chon, Seung-Hyun Feb 19, 2025 05:56am
- On the 18th, Celltrion announced that it had received marketing authorization from the European Commission for Stobocolo and Osenvelt, which are biosimilar versions of Prolia and Xgeva, respectively. The final approval was granted 2 months after the Committee for Medicinal Products for Human Use (CHMP) of the European Medicines Agency (EMA) recommended the products’ approval in December last year. Prolia and Xgeva are biopharmaceuticals developed by Amgen, and they were developed by varying the dose and dosing cycle of the main ingredient, denosumab. Prolia is used as a treatment for osteoporosis, and Xgeva has been approved for the prevention of bone complications in patients with bone metastases and the treatment of osteosarcoma. Based on the results of the global phase III clinical trial, Celltrion applied for approval of the 2 products, Stobocolo and Osenvelt, as biosimilars of the mentioned products in March last year. Stobocolo was approved for the treatment of osteoporosis and bone loss in postmenopausal women, while Osenvelt was approved for the prevention of bone metastasis complications in cancer patients and for treating giant cell tumors of bone. Celltrion received initial approval for the two products in Korea in November last year. It recently completed the application for the drug’s marketing authorization in the US as well. Major product groups that Celltrion is currently selling or has been approved for include: ▲Autoimmune disease treatment (Remsima, Remsima SC, Zymfentra, Yuflyma, Steqeyma, Aptozma), ▲anticancer drugs (Herceptin, Truxima, and Vegzelma), ▲ allergy treatment drugs (Omlyclo), ▲eye disease treatment drugs (Eydenzelt), and ▲bone disease treatment drugs (Stobocolo, Osenvelt). The market size of the 11 products totals approximately KRW 150 trillion. “With our existing products maintaining a strong market share in the European market, the approval of the additional follow-up products will further contribute to boosting Celltrion’s overall competitiveness.” said a Celltrion official.
- Company
- Osteonoic secures rights to J&J’s bone graft material
- by Lee, Seok-Jun Feb 19, 2025 05:56am
- Osteonic, a company specializing in implants for orthopedic surgery, announced on the 17th that it has secured the domestic rights to DBX Putty, a bone graft material, from Johnson & Johnson Medtech Korea. DBX Putty was developed by MTF Biologics Inc., a US bone graft manufacturer. Johnson & Johnson MedTech holds the global rights to the product, and Osteonic has secured the domestic rights through this agreement. DBX Putty is a DBM (Demineralized Bone Material) based bone graft. It is made by removing minerals from human bones and is used to reconstruct bone formation by implanting it into damaged bone parts or during spinal surgery. In particular, it has both osteoconductive and osteogenic functions because it is a mixture of mineral-removed cortical bone powder and highly biocompatible hyaluronic acid. This allows it to maintain the proper viscosity depending on the surgical situation and is highly regarded for its excellent osteogenesis and formability. Its quality has also been verified as a product that has been used in leading university hospitals and hospitals specializing in spinal joints in Korea for nearly 20 years. According to Fortune Business Insights, a global market research firm, the global market size of bone substitutes and bone grafts is estimated to be USD 5.7 billion (about KRW 7 trillion) in 2029, and about KRW 100 billion in Korea. Osteonic continues to grow by leveraging its full line-up of orthopedic implants that make up the human body, including Sports Medicine (soft tissue reconstruction), CMF (craniomaxillofacial), Trauma (upper and lower limb fractures), and Spine. Dong-won Lee, CEO of Osteonic, said, “Along with our existing business of treating fractures and spinal fixation implants, we plan to expand our business into the field of bone grafting materials through this licensing agreement and provide a wide range of musculoskeletal medical solutions.”
- Company
- Next reimb effort for 'Padcev combination therapy'
- by Moon, sung-ho Feb 19, 2025 05:56am
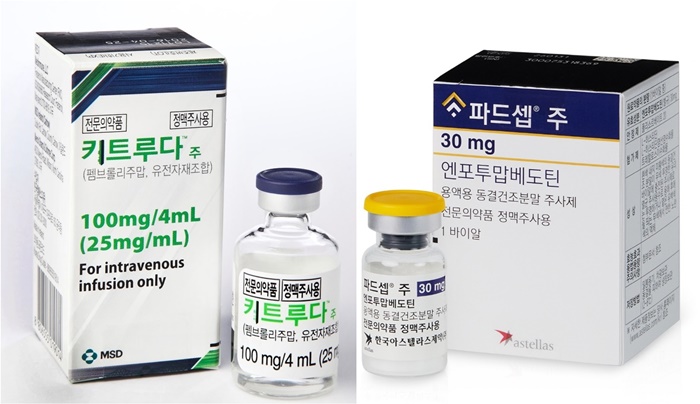
- 'Padcev Combination therapy' has been reported to have changed the urothelial cancer treatment paradigm after 30 years. After its launch in clinical practices in South Korea in the second half of last year, the government has initiated discussion for reimbursement of the therapy. Product photo of Keytruda and Padcev.According to the pharmaceutical industry on February 17, the Health Insurance Review and Assessment Service (HIRA) recently held the first Cancer Disease Review Committee (CDRC) for this year and discussed setting the reimbursement standards for the combination therapy containing Padcev (enfortumab, Astellas Pharma Korea) and Keytruda (pembrolizumab, MSD Korea). Padev was launched and became available for prescription in South Korea last year. It is an ADC anticancer agent for treating patients with metastatic urothelial carcinoma who failed previous treatments. In July 2024, indications were expanded as a first-line treatment in combination with Keytruda. Thus, Padcev is now an ADC anticancer agent approved for use in first-line to third-line treatments for metastatic urothelial carcinoma. Domestic approval was based on the EV-302 clinical study presented during the 2023 Congress of the European Society for Medical Oncology (ESMO Congress 2023). EV-302 is a randomized Phase 3 clinical study evaluating the effectiveness of Padcev+Keytruda combination therapy compared to platinum-based chemotherapy in 886 patients in 25 countries. Based on the study, at the median follow-up of 17.2 months, patients treated with Padcev combination therapy had a median overall survival (OS) of 31.5 months, extending the OS by approximately twofold compared to the platinum-based chemotherapy group and reducing death risk by 53%. The median progression-free survival (mPFS) of the combination therapy group was 12.5 months, and the mPFS of the platinum-based chemotherapy group was 6.3 months. The Padcev combination therapy extended the mPFS by approximately twofold. Based on this result, Astellas Pharma applied for reimbursement to the HIRA at the end of last year, and it has been considered for the first CDRC review for this year. However, the drug failed to pass the CDRC review after receiving the decision of 'reimbursement standards non-established.' Interestingly, Astellas Pharma had applied for reimbursement alone and its application was considered for the CDRC review. In the past, the review would have required applying for reimbursement with the Keytruda owner MSD. The policy has changed based on the global pharmaceutical companies' headquarters policy and the domestic‧foreign Fair Trade Act, and discussion with another pharmaceutical company can be considered 'price fixing.' As for Keytruda, which is used along with Padcev, MSD has not applied for reimbursement. It has been reported that MSD has applied for 17 indications, so the company may have been reluctant to file an additional one. However, the pharmaceutical industry believes that HIRA's approach toward combination therapies may have changed after the decision on the Padcev combination therapy. At the end of last year, HIRA announced the establishment of a review policy for reimbursement decisions on combination therapies. A pharmaceutical industry employee said who asked for anonymity said, "Last year, the CDRC review established a review policy for deciding on the reimbursement of combination therapies. However, the policy was limited to cases where a new drug is added to a previously reimbursed drug." He added, "The review of Padcev combination therapy indicates that an approach towards new drugs can be changed."
- Company
- Will Tevimbra become the 1st reimbursed immunooncology drug?
- by Eo, Yun-Ho Feb 19, 2025 05:56am
- Will the first immuno-oncology treatment option in the field of esophageal cancer finally be born in Korea? BeiGene Korea's immuno-oncology drug Tevimbra (tiselizumab), which passed the Health Insurance Review and Assessment Service’s Drug Reimbursement Evaluation Committee review last month, has entered into drug price negotiations with the National Health Insurance Service for insurance reimbursement. This comes about half a year after the drug passed the Cancer Disease Deliberation Committee review in August 2024 after a reattempt. Tevimbra is a PD-1 inhibitory immuno-oncology drug that has demonstrated clinical utility in second-line esophageal squamous cell carcinoma and was approved in Korea in November last year. Currently, there are seven immuno-oncology drugs approved and marketed in Korea: ▲Keytruda, ▲ Opdivo, ▲Tecentriq, ▲Imfinzi, ▲Bavencio, ▲Jemperli, and ▲Tevimbra, which have 64 indications. However, only 21 therapies (about 33%) are currently listed for reimbursement. None of these drugs are yet on the reimbursement list for esophageal cancer. Currently, only platinum-based chemotherapy is reimbursed in Korea as both first-line and second-line treatment options for esophageal squamous cell carcinoma. Reimbursement rates for immuno-oncology drugs by indication, including esophageal cancer, are low due to drug prices and national health insurance finances. Since the drugs were reimbursed for some cancers, such as lung cancer, the overall claims of immuno-oncology drugs and their share in health insurance finance expenditures have increased significantly, raising Korea’s financial burden. As of 2023, the total claims for anti-cancer drugs reached KRW 2.4 trillion, while claims for immuno-oncology drugs were KRW 500 billion, accounting for 20% of the total claims for anti-cancer drugs. This is why the industry is welcoming the news of BeiGene's initiation of drug price negotiations for Tevimbra, as the company has announced its intention to supply the drug at a relatively low price. BeiGene’s philosophy of providing “innovative new medicines at affordable prices” and eliminating underserved patients has already been demonstrated through the reimbursement process for its blood cancer drug Brukinsa (zanubrutinib). The company has also made Tevimbra available at no cost to select esophageal cancer patients through its compassionate use program (EAP, Expanded Access Program). It remains to be seen if Tevimbra will make it onto the reimbursement list after completing discussions with the Pharmacoeceonic Evaluation Subcommittee, Risk Sharing Subcommittee, and Drug Reimbursement Evaluation Committee. Tevimbra extended the median overall survival (OS) by 2.3 months compared to chemotherapy (8.6 months vs. 6.3 months) in the global Phase III RATIONALE-302 trial, statistically significantly reducing the risk of death by 30%. In the trial, Tevimbra demonstrated more than a twofold increase in the proportion of patients who responded to treatment compared to chemotherapy (20% vs. 10%), and the median duration of response was extended by about 3 months from 4.0 months to 7.1 months, showing a sustained response. Based on such results, the U.S. National Comprehensive Cancer Network (NCCN) recommended Tevimbra as a preferred option for the second-line treatment of esophageal squamous cell carcinoma at a high level (Category 1) in its revised treatment guidelines.
- Company
- Opdivo prolongs survival in urothelial carcinoma
- by Whang, byung-woo Feb 18, 2025 05:53am
- The emergence of new drugs such as immuno-oncology drugs in the first-line treatment of urothelial carcinoma, have refined treatment strategies in the area. With the number of options available in the clinical setting increasing, there is also growing concern over when and which treatment to select for the patients. However, experts believe that the choice of treatment that can maximize the effectiveness of the treatment is important, as the prognosis of urothelial carcinoma is still worse than that of other urologic cancers. Jong Jin Oh, Professor of Urology, Seoul National University Bundang Hospital Professor Jong Jin Oh, Professor of Urology at Seoul National University Bundang Hospital, who has the latest knowledge in the field, emphasized the need for institutional support for the emergence of new drugs that prolong the overall survival of patients with urothelial carcinoma. Urothelial carcinoma is a cancer that starts in the urothelial cells that line the inside of the bladder, and 90% of tumors that occur in the urinary tract are urothelial carcinoma. It is the most common type of bladder cancer, accounting for about 90% of all bladder cancer diagnoses. Even if patients undergo surgery, their life expectancy is not long, and the average overall survival period is just over one year, especially for patients with metastases. “In the first diagnosis, about 10% of patients with metastatic urothelial carcinoma are confirmed to have metastatic disease, and if adding patients whose cancer progressed or metastasized, 20-30% of all patients are confirmed to have metastatic disease,” said Professor Oh. “There may be microscopic metastases that are not detected by imaging tests, so the actual proportion of metastatic urothelial carcinoma may be higher than the confirmed proportion.” The chemotherapy combination of cisplatin and gemcitabine (GemCis) had been the representative treatment option. However, Professor Oh explained that the combination had clear limitations, such as response rate and toxicity. “The percentage of patients responding to gemcitabine is not high, and the duration of response is very short, less than a year, and the toxicity is strong, so patients cannot continue treatment for a long time,” said Professor Oh. ”Since urothelial carcinoma is a tumor that occurs in the urinary tract, many patients have reduced renal function, such as by having their kidneys or bladder removed.” The emergence of immune checkpoint inhibitors for urothelial carcinoma is expected to extend survival In this situation, the emergence of new drugs, including immune checkpoint inhibitors, is expected to extend patient survival. One of the recent changes is the approval of Opdivo (nivolumab) in combination with cisplatin and gemcitabine as a first-line treatment for unresectable or metastatic urothelial carcinoma in July. Looking at the Phase III CheckMate-901 trial, which was the basis for the approval of Opdivo, at a median follow-up period of 33.6 months, the median overall survival (mOS), the primary endpoint, was 21.7 months with the combination of Opdivo and chemotherapy, which was significantly longer than the 18.9 months with the combination of cisplatin and gemcitabine, and reduced the risk of death by 22%. “Opdivo is the first immuno-oncology drug approved for the first-line treatment of metastatic urothelial carcinoma. The combination of Opdivo and gemcitabine has extended the overall survival by about 3 months compared to the existing gemcitabine monotherapy,” said Professor Oh. ”This means that we have an opportunity to extend the expected life expectancy that has been around one year with the existing treatment to about one and a half years.” So, how has the actual prescription experience been for domestic patients? Professor Oh expected that Opdivo would play a role in the situation where most patients with metastatic urothelial carcinoma first experience lymph node metastasis. He said, “In the subgroup with lymph node-only metastases, the rate of complete remission of metastatic lesions was much higher with Opdivo than with gemcitabine therapy, and the duration was also much longer. As the study confirmed very good effects, I think it is an effective treatment that can be considered as a first-line treatment for patients with lymph node metastases. In fact, in the CheckMate-901 subgroup analysis, patients with lymph node-only metastases were compared between the combination of Opdivo and gemcitabine and Gemcitabine alone, and the median overall survival was 46.3 months for the combination of Opdivo and gemcitabine and 24.9 months for gemcitabine alone. In response, Professor Oh said, “Lymph nodes are where the immune response is most active in our bodies, so it is thought that their response rate to immuno-oncology drugs such as Opdivo will be high. Patients with cancer that has spread to other organs have a much lower level of activity, but patients with lymph node-only metastasis have a relatively good overall condition, which may have a positive impact on treatment outcomes as they can receive treatment as planned. In conclusion, in the first-line treatment of metastatic urothelial carcinoma, if the patient has a low tumor burden or lymph node metastasis alone, Professor Oh believes the relatively less toxic Opdivo-Gemcitabine regimen may be a useful option among the first-line treatment options. "Will increase Opdivo’s use in lymph node metastasis alone and as adjuvant therapy" In particular, Professor Oh focused on Opdivo’s use as adjuvant therapy based on the CheckMate-274 study. “Currently, the standard adjuvant therapy for urothelial carcinoma is GemCis, but there are cases where patients undergo surgery after chemotherapy and the results of the biopsy are not good. In this case, the effectiveness of adjuvant gemcitabine therapy is low, and the disease usually recurs within 6 months,” explained Professor Oh. “Since other therapies that can be tried outside of standard treatment for GemCis have not yet been established, this is a very unfavorable case, and we expect that the post-operative adjuvant therapy of Opdivo will be used most actively in such patients.” However, Opdivo as adjuvant therapy for urothelial carcinoma is not reimbursed by Korea’s health insurance. Professor Oh stressed the need for reimbursement of new drugs that can benefit patients with urothelial carcinoma, who have a short overall survival period and therefore are in urgent need of treatment. He said, “For patients with poor post-operative biopsy results, we are trying to use Opdivo as adjuvant therapy if conditions permit. Since there is no alternative to adjuvant Opdivo therapy, patients are very desperate so healthcare professionals believe the drug is absolutely necessary.” Finally, Professor Oh said, “The complete remission rate is about 40-50% with standard chemotherapy, but it can be improved to 60-70% with new drugs. I see the significance of its use as adjuvant therapy, and I hope that many patients will be able to use the drug without burden through prompt reimbursement.”
- Company
- Samsung Bioepis’s Prolia and Xgeva biosimilars approved
- by Chon, Seung-Hyun Feb 18, 2025 05:53am
- Pic of Samsung Bioepis Headquarters Samsung Bioepis' two bone disease treatment biosimilars have passed the US and European hurdles. Samsung Bioepis announced on the 16th that it has obtained marketing authorizations for its two biosimilar versions of Prolia and Xgeva, which are bone disease treatments, from the US Food and Drug Administration (FDA) and the European Commission (EC). Prolia and Xgiva are biopharmaceuticals developed by Amgen, and the two were developed by varying the dose and dosage cycle of the main ingredient, denosumab. Prolia is used as a treatment for osteoporosis, and Xgeva is approved for the prevention of skeletal system symptoms in patients with bone metastases and the treatment of giant cell tumors of bone. Last year, global sales of Prolia and Xgeva reached a total of USD 6.599 billion (KRW 9.7 trillion). Samsung Bioepis obtained separate marketing authorizations for each indication, just like the original drug. The Prolia biosimilar was licensed under the brand name Ospomyv in the US and Obodence in Europe. The Xgeva biosimilar was licensed under the name Xbryk in both the US and Europe. Samsung Bioepis has successfully commercialized 10 biosimilar products in the United States and 11 in Europe. A Samsung Bioepis official said, “We will continue to work to meet the unmet medical needs of patients around the world through the development of biosimilars in various disease areas.”
- Company
- Celltrion gains EU approval for Eylea biosimilar Eyedenzelt
- by Chon, Seung-Hyun Feb 17, 2025 05:53am
- On February 14, Celltrion announced that it had secured the marketing authorization for the Eylea biosimilar Eyedenzelt from the European Commission. Two months after receiving the recommendation for marketing authorization from the European Medicines Agency (EMA)'s Committee for Medicinal Products for Human Use (CHMP) in December, the drug was granted the final approval. Eyedenzelt is approved for the original drug's major indications to treat wet (neovascular) age-related macular degeneration (wAMD), retinal vein occlusion, diabetic macular edema (DME), and myopic choroidal neovascularization. In 2023, Eylea recorded sales of approximately KRW 13 trillion globally. Celltrion confirmed the equivalence of Eyedenzelt compared to the original drug based on the global phase 3 trials involving 348 patients with DME. Celltrion obtained approval from the Ministry of Food and Drug Safety (MFDS) in May and is currently working on the sales. In December, Celltrion received a recommendation from the EMA's CHMP for European marketing authorization of biosimilars, including Eyedenzelt, Actemra, Prolia, and Xgeva. Celltrion plans to expand its biosimilar portfolio to bone diseases and eye diseases, in addition to previously established autoimmune diseases and anticancer agents, through the approval of biosimilars, including Eyedenzelt. "Given the marketing authorization of Eyedenzelt, we can now expand product portfolio areas in the European market and speed up the launch in the global market," a Celltrion representative said. "As we expect to secure more approvals through the marketing authorization recommendation for biosimilars, Celltrion will strive to quickly launch the products and strengthen strategies to gain market dominance."